If you're a devoted side sleeper staring down a hysterectomy recovery timeline, you've almost certainly asked some version of this question — can you sleep on your side after a hysterectomy — either to your surgeon, to the internet at large, or quietly to yourself while mentally calculating how many weeks you'll be stuck on your back.
The good news: yes, you will sleep on your side again.
The more useful news: there's a thoughtful, evidence-based path to getting there safely, and preparing for that transition before surgery puts you significantly ahead of patients who figure it out as they go.
This guide covers everything you need to know about sleep positioning after a hysterectomy: why back sleeping is required early in recovery, when your surgeon will likely clear you for side sleeping, how to make that transition without setbacks, and what support tools make the difference between a smooth transition and a prolonged, interrupted one.
What Actually Happens to Your Body During a Hysterectomy?
Understanding why sleep positioning matters starts with understanding what your body is actually recovering from.
A hysterectomy is the surgical removal of the uterus. Depending on your diagnosis and treatment plan, it may also involve the removal of the cervix, ovaries, and fallopian tubes. It's performed for a range of conditions, including uterine fibroids, endometriosis, abnormal bleeding, uterine prolapse, and gynecologic cancers.
There are several surgical approaches:
Open (abdominal) hysterectomy involves a single larger incision in the lower abdomen. Recovery tends to be longer — typically six to eight weeks — with more significant internal healing required.
Laparoscopic or robotic-assisted hysterectomy uses several small incisions and specialized instruments, including the widely used da Vinci robotic system. This minimally invasive approach generally means less post-operative pain, shorter hospital stays, and faster return to normal activities — but it still involves real surgical trauma to abdominal tissues that requires careful positioning during recovery.
Vaginal hysterectomy removes the uterus through the vaginal canal without external incisions. Recovery is often the shortest of the three, but pelvic floor healing still places meaningful limits on early movement and positioning.
Regardless of approach, your body has just undergone major pelvic surgery. Muscles, fascia, ligaments, and abdominal structures have all been affected. That context is the foundation for everything that follows.
Why Can't You Sleep on Your Side Immediately After a Hysterectomy?
This is the part that frustrates natural side sleepers most, but the reasoning is sound.
In the first days and weeks following a hysterectomy, your abdominal and pelvic tissues are in active healing mode. The internal structures that were manipulated, cut, or repositioned during surgery need stable, low-pressure conditions to repair properly.
Side sleeping in early recovery creates several problems:
Pressure on incision sites. Even with laparoscopic surgery, the small abdominal incisions are healing from the inside out. Rolling to one side places direct or indirect pressure on those sites, which can disrupt healing tissue and increase discomfort.
Stress on the pelvic floor. Your pelvic floor has been under significant stress during surgery. Certain side-sleeping positions create twisting at the pelvis that strains structures that need rest.
Abdominal muscle activation. Getting into and out of a side-sleeping position requires your core and abdominal muscles — the very muscles doing most of the healing work — to engage in ways that flat-back positioning avoids.
Post-laparoscopic gas. Minimally invasive procedures use carbon dioxide gas to create surgical space inside the abdomen. That gas doesn't disappear immediately. Elevated back sleeping helps it dissipate. Side sleeping can trap it and intensify the shoulder and diaphragm discomfort that's already one of the more unpleasant post-laparoscopic surprises.
Drain management. Many hysterectomy patients have surgical drains in place for the first several days. Side sleeping can kink, compress, or dislodge drains — a complication nobody wants to manage mid-recovery.
How Long Before You Can Sleep on Your Side After a Hysterectomy?
Here's the answer you came for: with the honest caveat that your surgeon's guidance takes precedence over any general timeline.
For most hysterectomy patients, the general framework looks like this:
Days 1–7 (The Protected Phase): Back sleeping with the upper body elevated at 30–45 degrees is the standard recommendation by doctors and surgeons. This reduces swelling, supports circulation, manages gas discomfort, and protects incision sites from unnecessary pressure. Side sleeping is typically not recommended during this phase, regardless of surgical approach.
Weeks 2–3 (The Transition Window): Many patients with laparoscopic or robotic hysterectomies begin receiving clearance for careful, supported side sleeping around this point, provided healing is progressing well, gas pain has resolved, and there are no drain-related complications. Open hysterectomy patients typically remain in the protected phase longer.
Weeks 4–6: For open hysterectomy patients, this is often when side sleeping clearance begins. Laparoscopic patients may be largely back to their preferred position by this point, with supportive aids to cushion the abdomen.
Week 6 and beyond: Most patients receive full clearance for all comfortable sleep positions at or after their six-week follow-up appointment. Stomach sleeping is usually the last position to return.
These timelines are general guides, not medical guarantees. Every patient heals differently, and factors including age, BMI, surgical complexity, and overall health can shift these windows meaningfully. The single most important variable is your surgeon's individual assessment of your progress.
Does the Type of Hysterectomy Change the Sleep Positioning Rules?
Yes, meaningfully — though the principles remain consistent.
Laparoscopic and robotic hysterectomies typically allow earlier position flexibility because tissue trauma is more localized. The incisions are smaller and the internal disruption, while real, is less extensive than open surgery. Patients often find that supported side sleeping feels tolerable by the end of week two.
Open abdominal hysterectomy involves a more extensive incision and significantly more abdominal muscle disruption. The internal healing load is larger, and most surgeons recommend a longer period of elevated back sleeping before transitioning to other positions.
Vaginal hysterectomy has its own nuances. Without external abdominal incisions, the surface-level pressure concerns are reduced — but the vaginal and pelvic floor structures are doing substantial healing work, and positioning that strains the pelvis remains problematic in early recovery.
Total vs. partial hysterectomy can also affect recovery. Total hysterectomies (removing the uterus and cervix) involve more internal tissue than partial procedures, which may extend the window before full position freedom is appropriate.
When in doubt about where you fall on this spectrum, your surgeon's individual assessment of your healing is the most reliable guide.

What Sleeping Position Is Best in the First Weeks of Hysterectomy Recovery?
Elevated back sleeping is the therapeutic gold standard for the first phase of hysterectomy recovery, and it earns that designation for several interconnected reasons.
This isn't flat-on-your-back sleeping. At 30–45 degrees of upper body elevation:
Swelling is reduced. Elevation assists venous return, helping fluids move away from surgical sites rather than pooling around them.
Circulation improves. The elevated position reduces cardiac workload and supports blood flow to healing tissues.
Abdominal pressure decreases. Compared to lying completely flat, moderate elevation reduces the internal pressure on pelvic structures — a meaningful comfort factor in the first post-operative days.
Gas discomfort is minimized. For laparoscopic patients, elevation is the primary positioning strategy for managing residual CO2 gas, which gravitates toward the diaphragm and is referred to as shoulder and upper chest discomfort.
Getting in and out of bed is safer. The elevation reduces the distance and muscular effort required to sit up, which matters enormously when your abdominal muscles are recovering, and every movement needs to be deliberate.
The challenge most patients encounter is that achieving and maintaining this elevation throughout the night is harder than it sounds. A stack of household pillows creates an incline for approximately the first 20 minutes before gradually compressing and collapsing, leaving you without the support your body was relying on.

The Sleep Again Pillow System: Supporting Elevated Back Sleeping After a Hysterectomy
Elevated back sleeping isn't just a restriction to tolerate. It's an active part of your recovery. But achieving it consistently, night after night, requires more than a stack of household pillows. Elevation shifts during sleep, knee support collapses, and by 3am, you've lost the positioning your body needs.
The Sleep Again Pillow System was designed specifically for this phase. It combines an upper body wedge, leg support wedge, contoured side pillows, and a head pillow into a complete positioning system that holds the correct recovery posture throughout the night — not just when you first lie down.
What that means in practice:
- Upper body elevation at 30–45 degrees reduces post-surgical swelling and helps fluid drain away from pelvic tissue rather than pooling around healing structures
- Leg and knee support reduces abdominal wall tension, giving healing muscles and fascia the slack they need during the most critical repair window
- Contoured side pillows prevent unconscious rolling toward your side — the movement most likely to stress healing tissue before you're cleared for position changes
- The full system works together, which is what separates it from improvised setups that shift, flatten, or fail halfway through the night
For laparoscopic and robotic hysterectomy patients, elevation also addresses one of the more uncomfortable early-recovery surprises: residual CO2 gas from the procedure gravitates toward the diaphragm and is referred to as shoulder pain. The elevated position is your best tool for helping it dissipate.
The Sleep Again Pillow System is HSA/FSA eligible and ships fast from the USA and Canada. Everything can be in place before your procedure — not after you've already spent a week trying to solve your sleep setup while exhausted and in pain.
SHOP THE BEST SYSTEM FOR HYSTERECTOMY RECOVERY
What Are the Signs Your Body Is Ready for Side Sleeping?
Your surgeon's clearance is the primary authorization for position advancement, but your body also provides its own feedback worth paying attention to.
Generally, you're likely moving in the right direction when:
Incision tenderness has decreased significantly. When you can press gently near your incision sites without significant discomfort, healing has progressed to a point where light positional pressure is less problematic.
Gas discomfort has fully resolved. Residual post-laparoscopic gas typically clears within the first week for most patients. Attempting side sleeping while gas discomfort is still present often amplifies rather than relieves it.
You can change position without pain. The act of transitioning from your back to your side requires meaningful abdominal engagement. If that movement produces sharp or significant pain, your muscles are telling you something useful.
Drains have been removed. If you have surgical drains, their removal is generally a prerequisite before experimenting with side sleeping. Your surgeon or care team will confirm this timing.
None of these observations replace your surgeon's assessment — they're additional data points to bring to your follow-up conversations.

What Is the Safest Way to Transition Back to Side Sleeping After a Hysterectomy?
Moving from back sleeping to side sleeping after abdominal surgery is a gradual process that goes better with a deliberate approach.
Start with brief daytime trials. Before attempting side sleeping for a full night, test the position during daytime rest for 15–30 minute increments. This gives you calibrated feedback about what's comfortable and what needs more time.
Use a pillow for abdominal support. This is one of the most consistently recommended strategies by post-hysterectomy care teams. Place a pillow against your abdomen when side sleeping. This cushions any surface contact with your incision area, reduces the feeling of your abdominal contents shifting with gravity, and provides a comforting counter-pressure that many patients find significantly reduces discomfort.
Support behind your back as well. A pillow positioned behind you while side sleeping prevents unconscious rolling and gives your back muscles a resting surface, reducing the muscular work of maintaining a side position.
Bend your knees slightly. Gentle knee flexion while side sleeping reduces pelvic rotation and strain on the lower abdominal structures. A pillow between the knees takes this further by reducing hip and lower back strain.
Return to back sleeping without frustration. If side sleeping produces discomfort — even on the third or fourth week — returning to elevated back positioning for another few nights is a setback in the most minor sense. Your recovery timeline isn't permanently affected by waiting another few days before trying again.
Keep elevation available. Even as you transition toward side sleeping, maintaining the ability to return to elevated back positioning throughout the night is valuable. Having both positions supported means you can move between them as your body dictates.
What Support Do You Need When Side Sleeping During Hysterectomy Recovery?
The gap between what your body needs during the transition to side sleeping and what a pile of regular pillows can reliably provide is significant.
The primary needs are consistent abdominal support that cushions the incision area without creating pressure points, back support that prevents rolling and enables true side sleeping rather than a fatiguing half-propped position, and structural integrity that holds through the night without intervention. This is exactly where purpose-built support tools provide meaningful advantages over improvised alternatives.

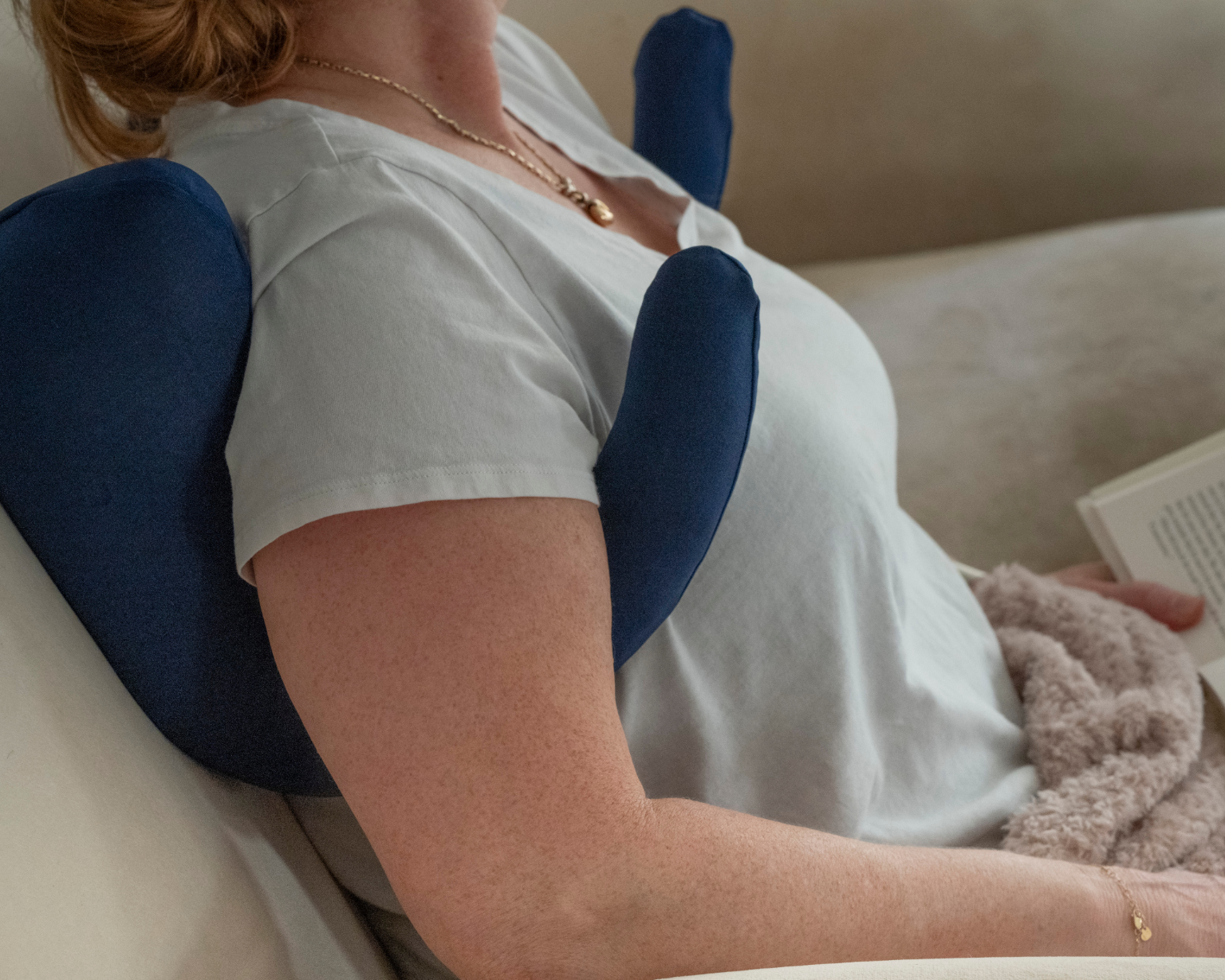
The Side Sleeping Chest Pillow: Built for the Transition Back to Side Sleeping
When your surgeon clears you for side sleeping, the challenge shifts. Your body has spent weeks in a protected position, and returning to your preferred sleep posture requires something most patients don't have ready: stable, consistent support against the abdomen.
That's the gap the Sleep Again Pillows Side Sleeping Chest Pillow fills.
This pillow was originally designed to support chest recovery patients during the side-sleeping transition. But patients quickly found other uses for it, including positioning it against the abdomen during side sleeping, which provides exactly the kind of support that freshly repaired abdominal tissue needs when transitioning off the back. For hysterectomy patients, it addresses the instability that makes early side sleeping uncomfortable: the sense that healing structures are shifting with gravity, unsupported and exposed.
What makes it different:
Adjustable width. The sides can be dialed in precisely to cradle the lower abdomen while simultaneously providing a resting surface for the back. You're not approximating the right setup with a folded pillow. You're placing support exactly where it needs to be.
Symmetrical design. Recovery sleep rarely looks like staying on one side all night — and it shouldn't. The symmetrical shape lets you turn freely from left to right without repositioning anything. For hysterectomy patients working toward even, unrestricted movement, this matters.
Structural integrity. This pillow holds its position through the night. That's not a minor detail during recovery. It's the difference between support that's actually there at 4am and support that's slid halfway down the mattress.
HSA/FSA eligible. The Side Sleeping Chest Pillow qualifies for HSA and FSA spending, making it a practical, reimbursable part of your recovery investment.
Ships fast from the USA and Canada. No waiting weeks for a package while you're already in recovery.
Please note: Due to federal regulations, bedding products are not returnable and all sales are final. Review product details at sleepagainpillows.com/products/side-sleeping-chest-pillow before purchasing.
For hysterectomy patients navigating the back-to-side-sleeping transition, this pillow belongs in your recovery plan.
SHOP THE BEST PILLOW FOR SIDE SLEEPING AFTER A HYSTERECTOMY
Can You Use HSA or FSA Funds for Hysterectomy Recovery Pillows?
Both the Sleep Again Pillow System and the Side Sleeping Chest Pillow qualify as HSA and FSA-eligible purchases for most plans.
HSA cardholders can typically use their card directly at checkout. FSA holders should submit documentation to their plan administrator for reimbursement. Ask your surgeon or care team about providing a letter of medical necessity, which strengthens your eligibility documentation. If you have questions about your specific plan, contact your administrator directly.
What Should You Prepare Before Hysterectomy Surgery for Better Sleep?
Recovery sleep quality correlates strongly with how well-prepared you are before surgery, not after. Patients who arrange their sleep setup in advance report smoother first-week experiences, better pain management, and more confidence navigating the early recovery period.
Talk to your surgeon about sleep positioning. Before your procedure, ask specifically:
What position will you recommend post-surgery for sleeping?
When do you typically clear patients for side sleeping?
Will I have drains, and how will that affect positioning?
What are the signs I'm healing on track for position advancement?
Set up your sleep space before you leave for the hospital. Post-surgery fatigue is real, and trying to arrange a support system when you're already exhausted and in pain is not the time to problem-solve. Have your positioning tools in place and tested before the day of surgery.
Plan the transition, not just the beginning. Most hysterectomy recovery sleep guides focus entirely on the first two weeks. But the transition to side sleeping — weeks two through six for most patients — is often where the real sleep disruption happens. Preparing for that phase specifically, including having the right support tools ready, puts you ahead.
Tell your household what to expect. If you share a bed, your partner needs advance notice about temporary adjustments to the sleep setup. The earlier that conversation happens, the less friction there is during the recovery period itself.
Practice the positions before surgery. This sounds unusual, but spending a night or two in an elevated back-sleeping position before your procedure accomplishes two things: it identifies any comfort adjustments needed in your setup, and it gives your nervous system a reference point so the position feels less foreign when it becomes mandatory.
What Else Should You Know About Hysterectomy Sleep Recovery?
Pain management affects positioning. Post-surgical medications affect your awareness of positioning-related discomfort. As medications taper, you may become more aware of position-related sensations that were masked earlier. This isn't regression — it's your body providing more accurate feedback about where it is in healing.
Healing isn't linear. A day that feels like a step backward is usually just a day. The overall trajectory of hysterectomy recovery is reliably forward; individual days don't define the arc.
Your preferred pre-surgery sleep position will return. Side sleepers who spend six weeks on their backs overwhelmingly return to their preferred position once cleared. The temporary displacement is real and frustrating, and it's temporary.
Here's the Plan
Can you sleep on your side after a hysterectomy? Yes, but not initially, and the timing depends on your surgical approach, your individual healing, and your surgeon's specific guidance.
The informed approach is this: protect your recovery with recommended elevated back sleeping in the early weeks, use the right tools to maintain therapeutic positioning throughout the night, and prepare for the transition to side sleeping so that when clearance comes, you're ready to move smoothly and comfortably into it.
The best time to prepare your recovery sleep setup is before you need it.
Important Medical Disclaimer
The information provided on this page is for educational purposes only and should not replace professional medical advice from your healthcare provider. Sleep Again Pillows are positioning support products designed to help maintain sleep positions recommended by medical professionals during recovery and for therapeutic use.
Always follow your surgeon's or physician's specific post-operative instructions and positioning requirements. Medical guidance from your healthcare team takes precedence over any general information provided here. Recovery timelines, positioning angles, and product suitability vary based on individual surgical procedures, medical conditions, and patient-specific factors.
Consult your healthcare provider before purchasing positioning equipment if you have specific medical concerns or questions about whether these products are appropriate for your recovery or medical condition(s). Your medical team can provide personalized recommendations based on your unique situation.
Sleep Again Pillows do not diagnose, treat, cure, or prevent any medical condition. These products provide positioning support to help maintain sleep angles and positions as directed by your healthcare provider.