How you sleep after your breast lift matters as much as anything else you'll do during recovery, and the best time to prepare for it is right now, before you ever walk into the operating room.
Sleep isn't passive recovery. It's active healing. While you're unconscious, your body is cycling through repair processes, releasing growth hormone, managing inflammation, and delivering oxygen-rich blood to healing tissue. Your sleep position either supports that work or actively undermines it. After a breast lift, the wrong position puts pressure on fresh incisions, disrupts lymphatic drainage, and can compromise your results. The right position — elevated back sleeping as recommended by doctors and surgeons — makes those same hours work actively toward your recovery.
This guide will walk you through everything you need to know about sleeping after a breast lift, with the emphasis on preparing before surgery so you're not improvising in the middle of Week One.
What Happens to Your Body During a Breast Lift?
A breast lift (mastopexy) removes excess skin, repositions the nipple-areola complex, and reshapes the breast tissue to create a lifted, more youthful contour. Depending on your anatomy and goals, your surgeon may use a periareolar (donut), vertical (lollipop), or anchor (inverted-T) incision pattern. In some cases, a breast lift is combined with augmentation to restore volume.
Regardless of the specific technique, the post-surgical reality is the same: your chest tissue has been lifted, reshaped, and sutured. Your body immediately begins the inflammatory healing response — swelling, bruising, and fluid accumulation are expected and normal. Your incisions need protection from pressure and tension. Your lymphatic system needs to drain efficiently. Your circulatory system needs uninterrupted access to healing tissue.
Every one of these processes is either helped or hindered by where you put your body during the hours you spend sleeping.

Why Is Elevated Back Sleeping the Gold Standard After a Breast Lift?
Plastic surgeons consistently recommend the same position for breast lift patients: on the back, with the upper body elevated at 30 to 45 degrees. This isn't just clinical preference. T's physics, physiology, and anatomy working together.
What Does Elevation Actually Do?
Reduces Swelling Through Gravitational Drainage
Swelling after a breast lift is caused by fluid accumulating in the tissue as part of the inflammatory response. Your lymphatic system is responsible for clearing that fluid, and it relies heavily on gravity to do its job. When your upper body is elevated, lymphatic fluid drains downward and away from your chest rather than pooling around your incisions. Reduced swelling means less pressure on healing tissue, less discomfort, and a faster return to the results you came for.
Protects Incisions from Pressure and Tension
Lying completely flat puts your incisions in contact with the mattress and creates direct pressure on sutured tissue. Even small amounts of sustained pressure on healing incisions can interfere with normal closure, increase scarring, and cause unnecessary discomfort. Elevation keeps your chest lifted off the sleep surface, distributing body weight across your back rather than concentrating it at the surgical sites.
Improves Circulatory Efficiency
Your cardiovascular system is working overtime post-surgery, delivering oxygen and nutrients to healing tissue while clearing away inflammatory byproducts. Elevating your upper body reduces the work your heart has to do, improving the overall efficiency of blood delivery to your chest. Better circulation means faster tissue repair and reduced inflammation.
Enhances Breathing Comfort
Post-surgical chest tightness, swelling, and the natural discomfort of incision sites can make deep breathing feel labored. Elevated positioning opens the airways, allows the diaphragm to work more efficiently, and reduces the feeling of pressure on the chest wall. This isn't just about comfort. Adequate breathing after surgery helps prevent complications like fluid accumulation in the lungs, and deeper breathing promotes the kind of restorative sleep cycles that accelerate healing.
Makes Getting Up Safer and Easier
Rising from a flat position requires significant engagement of your core and chest muscles, exactly the muscles you're trying to protect after a breast lift. From an elevated position, you work with gravity rather than against it, reducing the strain on your incisions every time you need to get up for water, medication, or a bathroom trip. Over the course of a week with multiple nightly disruptions, this mechanical advantage adds up.
Why Does the 30-45 Degree Angle Matter for Breast Lift Recovery?
Not all elevation is created equal. Here's what the numbers mean in practice:
Under 30 degrees provides insufficient drainage and doesn't offer meaningful rolling resistance. This range is essentially tilted flat. It looks like elevation, but doesn't deliver therapeutic benefit.
30-45 degrees is the therapeutic window. At this angle, your upper body is stable enough to remain in position throughout a full night without constant readjustment, while still delivering meaningful drainage and pressure relief. Most surgeons recommend staying within this range for the first two to four weeks of recovery.
Above 45 degrees begins to create its own problems. Neck strain, hip pressure, and the tendency to slide down during the night, which causes involuntary movement that can disturb healing tissue.
The 30-45 degree range is not arbitrary. It represents the intersection of physiology and comfort — therapeutic enough to support healing, sustainable enough to actually maintain through a full night of sleep.

Why Should You Prepare Your Sleep Setup Before Breast Lift Surgery?
Here's the part most recovery guides skip entirely: you can, and should, start sleeping in your recovery position weeks before your procedure.
If you're a side sleeper or stomach sleeper, back sleeping will feel foreign at first. Your body has years of established muscle memory telling it to rotate into its preferred position, and it will try to reassert itself while you're fully unconscious.
The solution is pre-surgical training:
Practice elevated back sleeping 2-4 weeks before your procedure. Your body needs time to adapt to a new position before it becomes the default during sleep. Starting early means you'll arrive at your procedure date already comfortable with the position — not learning it while also managing pain, medication, and recovery.
Set up your sleep system before surgery day. Arriving home after surgery is not the moment to work out your pillow configuration. Have your support system assembled and tested before your procedure.
Identify your barriers. If you consistently wake up on your side, you'll need physical deterrents — pillows, rolled blankets, or a purpose-built positioning system — to prevent unconscious rolling. Test these before surgery so you know what works for your body.
Create the conditions for quality sleep. Limit caffeine after mid-afternoon, avoid screens in the hour before bed, and aim for a consistent sleep schedule in the weeks leading up to your procedure. Good pre-surgery sleep habits compound into better post-surgery recovery.

What About Side Sleeping After a Breast Lift?
Side sleeping is recommended immediately after a breast lift, but it's worth addressing honestly because many patients find it impossible to avoid completely.
The core problem with side sleeping after a breast lift is asymmetrical pressure. When you roll onto one side, your upper arm rests against your chest, and your breast tissue is compressed between your arm and the mattress. For freshly sutured tissue, that pressure can cause discomfort, disrupt healing, and potentially affect your final results. If you've had implants placed alongside your lift, the stakes are even higher — lateral pressure can interfere with implant settling and shift positioning before adequate scar tissue has formed to hold things in place.
Most surgeons restrict side sleeping for at least the first four to six weeks, with the earliest clearance for modified side sleeping coming only with substantial chest support. Week 6 and beyond is when most patients receive broader position clearance, though this varies by procedure and individual healing.
Always confirm your specific timeline with your surgeon. Healing varies by person, procedure complexity, and individual factors — don't self-advance to side sleeping before your provider has cleared you.
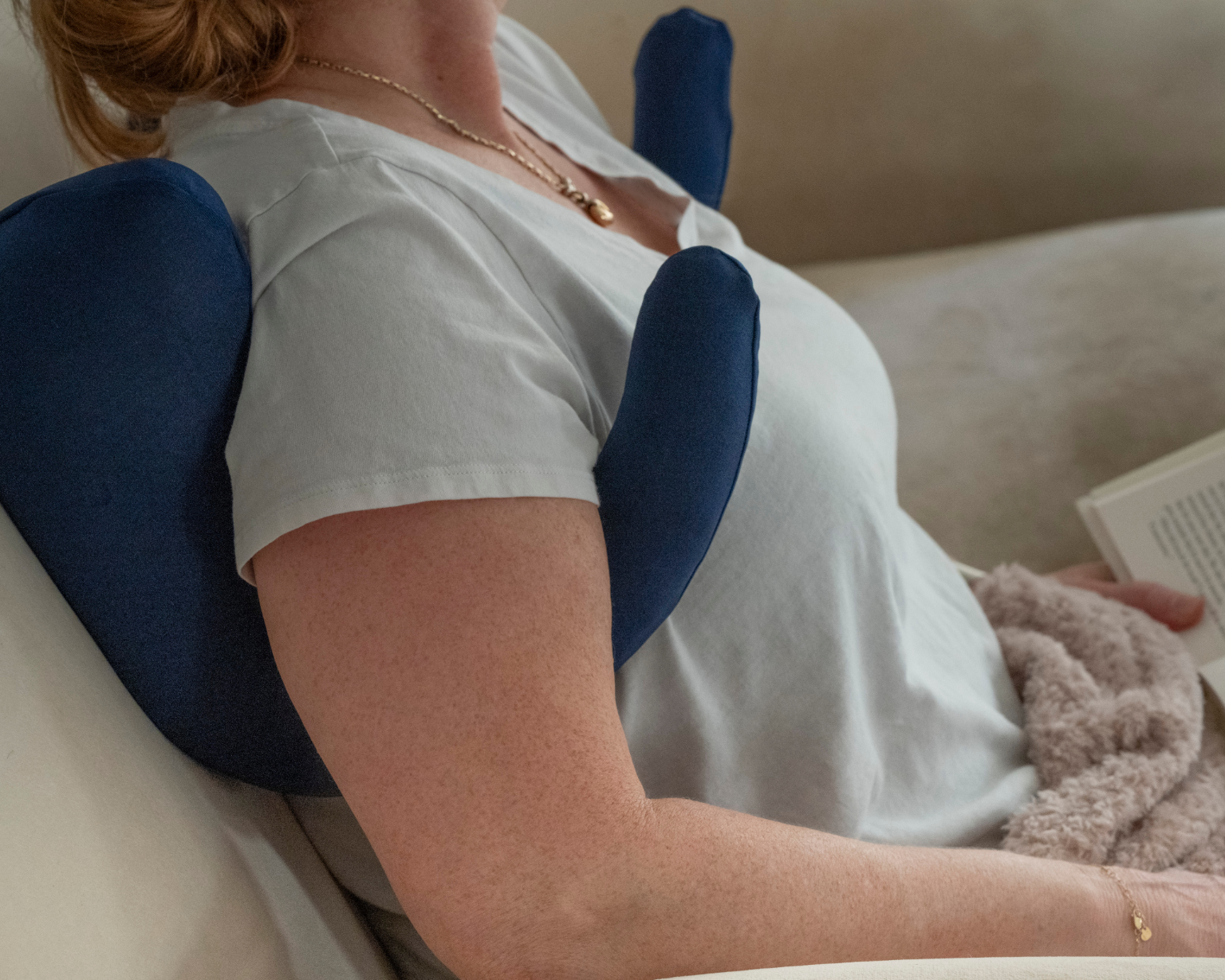
When you are cleared to transition to side sleeping, support matters enormously. The Side Sleeping Chest Pillow was specifically designed for this transition. Its adjustable-width, U-shaped design cradles the chest from both sides simultaneously, reducing direct pressure on healing tissue while also supporting the back. The symmetrical design allows you to turn freely to either side during the night without repositioning. Continue sleeping in your compression bra and position a firm pillow behind your back to prevent full rollover until you're fully cleared.
What Does a Week-by-Week Sleep Strategy Look Like After a Breast Lift?
Before Surgery: Foundation Phase
Preparation done here pays the biggest dividends during recovery. Get your positioning system set up and ready before your procedure date. Your goal is to make the first post-op night as friction-free as possible. See the Pre-Surgery Sleep Setup Checklist below for the full rundown.
Week 1: Maximum Elevation and Protection
This is your most critical week. Elevation at 30-45 degrees delivers maximum swelling management when you need it most. Pain medication and the lingering effects of anesthesia can cause position shifts without awareness. Physical barriers are essential for preventing rolling onto healing tissues. Prioritize sleep quality over comfort preferences. This phase is temporary; your results are permanent.
Weeks 2-3: Consolidation
Swelling typically peaks between days 2-4 and begins to diminish. Most patients find their rhythm during this phase and report improved sleep quality as acute post-surgical discomfort decreases. Maintain your back-sleeping discipline, and do not test side sleeping yet, until cleared by your surgeon.
Weeks 3-4: Monitoring and Refinement
Continue protective positioning while watching for improvements. Notice whether elevated positioning has started to feel natural. Many patients find it does. Your compression bra continues to provide important support during sleep throughout this phase.
Week 4-6: Surgeon-Guided Transition
At your follow-up appointments, your surgeon will assess healing progress and advise when modified side sleeping may be appropriate. Begin any position transitions gradually and with full support in place.
Week 6+: Clearance-Based Freedom
Most patients receive general position clearance around 6-8 weeks, though individual timelines vary. Back sleeping will likely feel more natural by this point than it did when you started. Many patients continue the practice long after medical necessity ends.
What Are the Most Common Sleep Positioning Mistakes After a Breast Lift?
Even well-intentioned patients make a few consistent mistakes during breast lift recovery:
Underestimating the elevation angle. Anything under 30 degrees doesn't deliver meaningful therapeutic benefit. If you're stacking pillows, measure or estimate your angle honestly — feeling "slightly tilted" usually means you're well below the therapeutic threshold.
Relying on willpower instead of physical barriers. You cannot consciously control sleep position while unconscious. If you're a habitual side sleeper, the question is not whether your body will try to roll — it's whether you've made rolling physically difficult enough to prevent it.
Abandoning elevation too early. The instinct to return to flat sleeping once the acute pain subsides is understandable, but healing continues well beyond the point where you stop feeling it. Follow your surgeon's timeline, not your comfort level.
Ignoring leg support. Elevated upper-body positioning without leg support can create lower back strain that compounds over days and weeks. A leg support wedge keeps spinal alignment intact across the full body, not just from the waist up.
Why Do DIY Pillow Setups Fall Short for Post-Surgical Recovery?
The instinct to stack a few bed pillows and call it a recovery setup is understandable, but it creates predictable problems.
Regular pillows compress under body weight. A stack that starts at 40 degrees of elevation can lose most of its height over the course of a night, dropping well below the therapeutic range without any obvious indication. Individual pillows also shift, separate, and develop gaps — gaps that create uneven pressure points precisely where you don't want them. Restoring a collapsed pillow setup while in discomfort disrupts sleep and works against the recovery process.
Effective post-surgical sleep positioning requires an engineered approach: stable elevation that holds its angle through hours of sleep, integrated support across the full body, and barriers that remain in place whether you're conscious or not.

The Sleep Again Pillow System: Engineered for Breast Lift Recovery
The Sleep Again Pillow System was designed specifically to solve the positioning challenges that come with breast lift recovery. It includes everything you need, ready to go before your procedure date.
Every Sleep Again Pillow System includes:
-
Two Contoured Side Pillows to cradle the back and hips and create physical barriers against unconscious rolling
-
Upper Body Wedge to create the optimal upper body incline within the therapeutic 30-45 degree range
-
Leg Support Wedge to gently elevate the legs and maintain full-body spinal alignment
-
Head Pillow to provide head support and neck mobility at therapeutic angles
-
Removable, washable slipcovers for every piece — because recovery takes weeks, and hygiene during extended use matters
The Upper Body Wedge maintains its incline through a full night of sleep without compression or collapse. The Contoured Side Pillows provide consistent resistance against rolling, not just the first hour, but all night. Because each component is designed to work with the others, there are no gaps, no shifting, and no middle-of-the-night readjustment sessions.
The Sleep Again Pillow System is also HSA/FSA eligible. That makes it a practical pre-surgery purchase that eliminates guesswork on day one of recovery.
Please note: as bedding products, all Sleep Again Pillow System sales are final per federal regulations governing bedding items.
SHOP THE BEST PILLOW FOR BREAST LIFT RECOVERY

Pre-Surgery Sleep Setup Checklist
Before your breast lift date, confirm you have:
-
Your post-surgery pillow system, assembled and tested
-
Fresh linens washed and ready. The Sleep Again Pillow System has a bundle option that includes a custom fitted sheet, and there's now a second cooling fitted sheet option.
-
Compression bra sized and accessible for night use
-
Pain medication prescription filled and within reach of your bed
-
Water and any nighttime essentials nearby with easy access without a full sit-up
-
A practice run of 3+ nights sleeping in your recovery position
The patients who sleep best during breast lift recovery are the ones who treated their sleep setup with the same intentionality they gave to choosing their surgeon.

When You're Ready to Transition: Side Sleeping After a Breast Lift
Elevated back sleeping gets you through the critical weeks. But for the majority of patients who were side sleepers before surgery, the question eventually becomes: when can I sleep on my side after a breast lift?
The challenge with side sleeping after a breast lift isn't just timing — it's mechanics. When you roll onto one side, your upper arm presses against your chest, and your breast tissue compresses between your arm and the mattress. For tissue that has been lifted, reshaped, and sutured, that asymmetrical pressure is exactly what you spent weeks protecting against. The transition back to side sleeping needs to be supported, not improvised.
That's what the Side Sleeping Chest Pillow was designed for.
Its adjustable-width, U-shaped design cradles the chest from both sides simultaneously, reducing direct pressure on healing tissue while supporting the back to prevent a full rollover.
Unlike propping a standard pillow against your chest, the symmetrical design means you can turn to either side during the night without waking up to reposition. Support stays consistent whether you start the night on your left or your right.
A few principles for the transition:
- Wait for your surgeon's clearance. Most patients receive the go-ahead for modified side sleeping around weeks 4–6, depending on healing progress. Don't self-advance this timeline.
- Keep your compression bra on. Your surgeon will advise when you can discontinue nighttime bra use. Until then, it continues to provide important structural support during sleep.
- Go gradually. Your first nights of side sleeping may be shorter stints rather than a full night. That's normal. Let your comfort — and your surgeon's guidance — lead the pace.
Q&A: Sleeping After a Breast Lift
How long do I need to sleep elevated after a breast lift?
Most surgeons recommend elevated back sleeping for at least the first two to four weeks following surgery. The exact duration depends on your specific procedure, how you heal, and your surgeon's assessment at follow-up appointments. Many patients continue elevated back sleeping beyond the mandatory period because they find it genuinely improves their rest.
Can I sleep on my side at all after a breast lift?
Not during the initial recovery phase. Side sleeping puts direct pressure on healing breast tissue and incisions and should be avoided for at least four to six weeks. Your surgeon will advise you on when you can begin transitioning back to side sleeping.
When that transition does come, the Side Sleeping Chest Pillow is purpose-built for exactly this moment. It cradles the chest from both sides with an adjustable-width design that takes direct pressure off healing tissue. If you've had implants placed alongside your lift, your timeline may be longer.
What happens if I accidentally roll onto my side during sleep?
One instance of rolling is unlikely to cause serious harm, but it will likely wake you up uncomfortably. The greater concern is repeated unconscious rolling, which is why physical barriers — not willpower — are the appropriate prevention strategy. If you find yourself consistently waking on your side, your positioning setup needs reinforcement.
Is sleeping in a recliner a good option after a breast lift?
A recliner can be a good option for resting and napping during the day, but it doesn't usually achieve the same meaningful sleep as you would get in your own bed. Plus, medical recliners are expensive to rent and challenging to maneuver into your home.
Why do my household pillows keep collapsing during recovery?
Standard pillows are designed for comfort, not for maintaining a specific therapeutic angle under sustained body weight. They compress and shift during the night, gradually reducing the elevation that provides medical benefit. For multi-week recovery positioning, that inconsistency creates real problems for both sleep quality and healing.
Can I use my HSA or FSA to purchase a post-surgical sleep positioning system?
Yes, in some cases. Post-surgical positioning products, including the Sleep Again Pillow System, are HSA/FSA eligible because they serve a direct medical recovery function. This is worth factoring into your pre-surgery planning. Purchasing before your procedure means your system is ready and waiting when you need it most.
When can I sleep on my stomach again after a breast lift?
Stomach sleeping is generally off-limits for the entire recovery period. Most surgeons require a full 8-12 weeks before any return to stomach sleeping, and some advise against it indefinitely following breast augmentation with lift due to implant positioning considerations. Follow your surgeon's specific guidance carefully on this point.
Will I always need to sleep on my back after a breast lift?
No. The elevated back sleeping requirement is temporary and tied specifically to the healing phase. Once your surgeon provides clearance — typically around the 6-8 week mark — you can gradually return to your preferred positions. Some patients discover during recovery that elevated sleeping improves their general sleep quality and choose to continue it voluntarily, but it is not a permanent requirement.
Important Medical Disclaimer
The information provided on this page is for educational purposes only and should not replace professional medical advice from your healthcare provider. Sleep Again Pillows are positioning support products designed to help maintain sleep positions recommended by medical professionals during recovery and for therapeutic use.
Always follow your surgeon's or physician's specific post-operative instructions and positioning requirements. Medical guidance from your healthcare team takes precedence over any general information provided here. Recovery timelines, positioning angles, and product suitability vary based on individual surgical procedures, medical conditions, and patient-specific factors.
Consult your healthcare provider before purchasing positioning equipment if you have specific medical concerns or questions about whether these products are appropriate for your recovery or medical condition(s). Your medical team can provide personalized recommendations based on your unique situation.
Sleep Again Pillows do not diagnose, treat, cure, or prevent any medical condition. These products provide positioning support to help maintain sleep angles and positions as directed by your healthcare provider.