If you're finding sleep challenging after your lumpectomy, know that you're not alone in this experience. Many people find that while the surgery itself may be straightforward, figuring out how to rest comfortably afterward presents unexpected challenges.
You might recognize this scenario: you're feeling positive about your recovery progress during the day, but when bedtime arrives, finding a comfortable position becomes surprisingly difficult. The surgical area may be tender, and your usual sleeping positions might not feel quite right anymore.
The good news is that with some thoughtful adjustments to your sleep setup and positioning, you can find comfort again. This isn't about enduring weeks of poor sleep—it's about making strategic changes that support your healing while helping you rest well.
Your body has been through something significant, and it deserves the restorative sleep that aids recovery. Let's work together to create a sleep environment that feels supportive and comfortable, so you can focus your energy on healing rather than on solving bedtime comfort puzzles.
Why Lumpectomy Sleep Recovery Feels Like Mission Impossible
Let's start with some truth-telling: lumpectomy recovery sleep challenges aren't in your head, and you're not being dramatic. Your body just went through a surgical procedure that affected one of the most movement-sensitive areas of your anatomy. Every time you shift, reach, or even breathe deeply, you're reminded that things are not quite back to normal.
Sufficient rest isn't just helpful after your lumpectomy—it's absolutely essential. Your body becomes a healing machine during sleep, but only if you position yourself correctly. Getting this right means the difference between a smooth recovery and playing twenty questions with your comfort level every night.
The anatomy of lumpectomy sleep problems:
Incision protection mode: Your surgical site needs to heal, which means avoiding pressure, stretching, or any movement that could stress the healing tissue. Unfortunately, this eliminates about 90% of your normal sleep positions.
Arm and shoulder compensation: When you can't move normally on your surgical side, your body starts compensating with awkward positioning that creates new discomfort in your neck, shoulder, and back.
The drainage situation: If you have surgical drains, you're essentially sleeping with medical tubing that needs to be positioned carefully without pulling or kinking—an added complication to your sleep setup.
Movement anxiety: Even when you're comfortable, there's the constant worry about rolling onto your surgical side during sleep. Your brain stays partially alert, preventing the deep rest you desperately need for healing.
The Lumpectomy Sleep Position Hierarchy: From "Absolutely Not" to "Actually Doable"
Position Level 1: The Forbidden Zone (Don't Even Think About It)
Stomach sleeping: This position is completely off the table for the foreseeable future. The pressure on your surgical site would be like asking your wound to enjoy unwanted pressure.
Surgical side sleeping: Rolling onto your affected side puts direct pressure on the incision and can disrupt the healing process. Save this position for much later in your recovery when your surgeon gives the all-clear.
Position Level 2: Proceed with Extreme Caution
Non-surgical side sleeping: Your non-operated side becomes neutral territory that most patients can navigate without issues. This can work with proper support, but requires strategic pillow placement to prevent you from unconsciously rolling toward your surgical side during sleep.
Flat back sleeping: While better than the forbidden positions, lying completely flat often doesn't provide enough elevation for optimal healing and can make it harder to get up when you need to move.
Position Level 3: Your New Best Friends
Elevated back sleeping: This becomes your sleep recovery headquarters—the position that makes everything else possible. Picture yourself in a comfortable reclined position that happens to be your bed, angled just right to let gravity work in your favor instead of against you. This position minimizes strain on healing tissue while reducing swelling and making those inevitable middle-of-the-night bathroom trips significantly easier.

The Elevated Back Sleep Setup: Your Recovery Command Center
Elevated back sleeping isn't just a good option for lumpectomy recovery—it's usually the position that makes everything else possible. This position reduces pressure on your surgical site, improves circulation, minimizes swelling, and makes it easier to get up for those inevitable middle-of-night bathroom trips.
Why Regular Pillows Fail at This Job
Here's the brutal truth about using random household pillows for lumpectomy recovery positioning: they're completely unreliable. Regular pillows compress under body weight, shift during normal sleep movement, and lose their therapeutic positioning exactly when you need support most.
You end up spending 15-20 minutes each night playing pillow arrangement games, only to wake up at 3 AM when everything has collapsed and you're back to square one. This constant repositioning disrupts your sleep cycles and interferes with the deep sleep your body needs for healing.
Creating the Perfect Elevation Angle
Most lumpectomy patients find the 30-45 degree range to be their optimal angle—steep enough to provide real therapeutic benefits, gentle enough that you don't feel uncomfortable. You can achieve this angle with a reclining chair or strategic pillow arrangement, though quality positioning systems like the Sleep Again Pillow System eliminate the guesswork and nightly setup frustration.
Start higher, go lower: Begin with 40-45 degrees in the first few days when swelling is at its peak, then gradually reduce the angle as healing progresses and comfort improves.
The Architecture of Comfort
Base support: Use a quality wedge pillow or carefully arranged firm pillows to create stable elevation that won't compress and lose its angle during sleep.
Arm positioning: Your surgical side arm should be supported at a natural angle—not hanging off the side, not pressed against your body, but comfortably resting in a neutral position.
Non-surgical side support: Create a barrier with pillows to prevent unconscious rolling toward your affected side during sleep.
Getting out of bed becomes exponentially easier from an elevated position—you're working with gravity instead of fighting it, which means less strain on your healing surgical site during those necessary position changes.
SHOP THE BEST PILLOW FOR LUMPECTOMY RECOVERY
Strategic Side Sleeping: When Back Sleeping Needs a Break
While elevated back sleeping should be your primary position during early lumpectomy recovery, there will be times when you need positional variety or when back sleeping simply isn't working for you.
Non-Surgical Side Sleeping Setup
Create a comprehensive support system that prevents rolling while maintaining comfort. This isn't just about throwing a pillow behind your back—it's about creating barriers that work unconsciously.
Surgical side protection: Use a firm pillow or body pillow against your surgical side to create a buffer zone. This pillow should be positioned to support without putting any pressure on your incision area.
Back barrier: Place a substantial pillow behind your back to prevent unconscious rolling toward your surgical side during sleep.
Arm support: Your surgical side arm needs somewhere comfortable to rest that doesn't create strain. Use pillows to create a "nest" where your arm can rest naturally.
The Recovery Progression
Most surgeons recommend prioritizing elevated back sleeping for several weeks, but the timeline varies based on your specific surgery and healing response. Here's the typical progression:
-
Week 1: Elevated back sleeping is your primary residence, with minimal side sleeping adventures
-
Week 2: Carefully introduce longer periods of non-surgical side sleeping when comfort allows
-
Week 3-4: Gradually increase side sleeping duration while monitoring your body's feedback
-
Week 4+: Begin discussing surgical side sleeping with your surgeon—but only with their explicit approval

Managing Drains and Sleep Bras
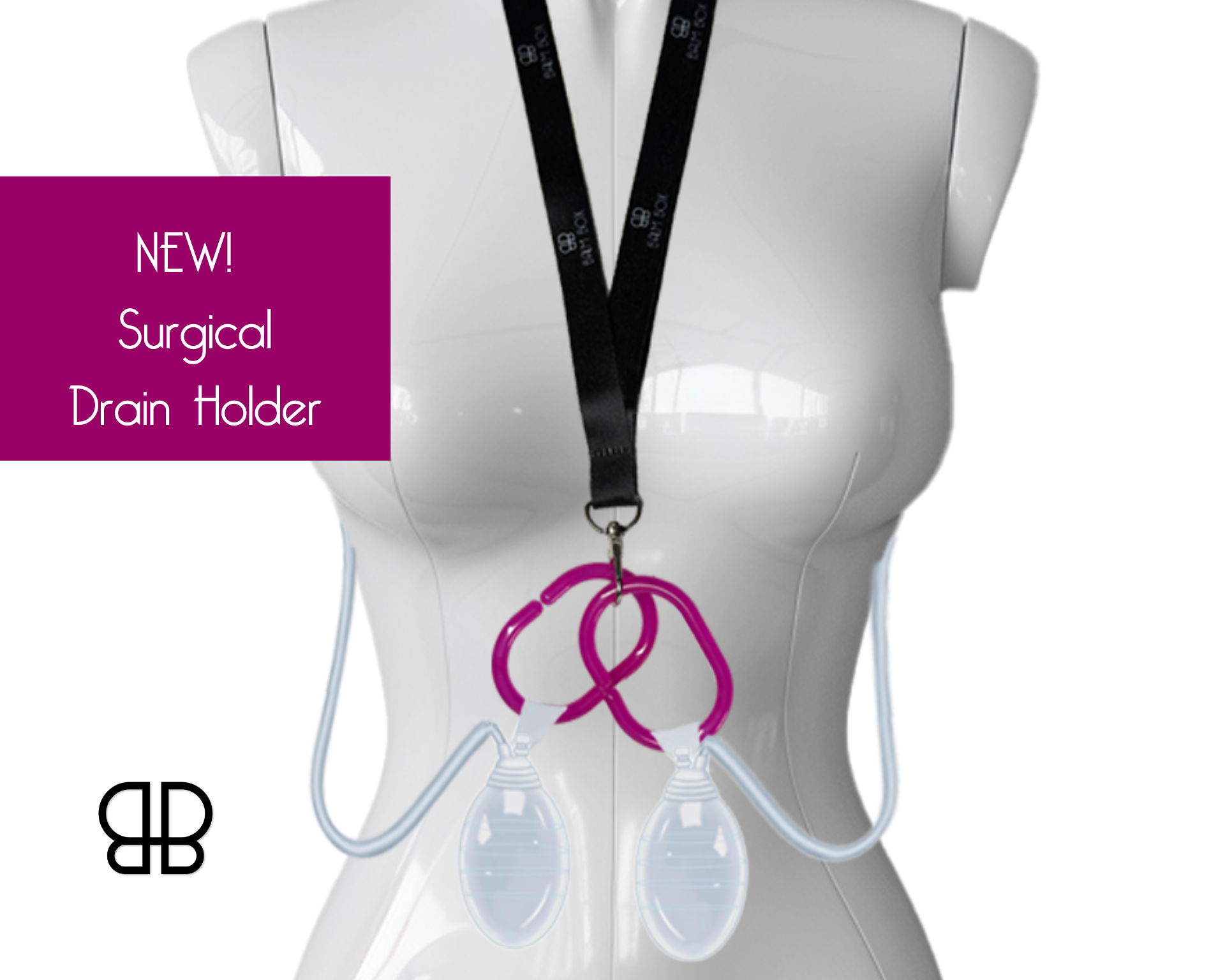
If you have surgical drains, sleeping becomes an exercise in medical tube management. These drains are crucial for healing, but they turn every position change into a careful choreography.
Drain positioning strategies:
-
Create a drainage station next to your bed where drains can rest without pulling or kinking
-
Wear a surgical drain holder or specialized post-surgical garment to keep drains secure
-
Ensure tubing has enough slack to accommodate normal sleep movement
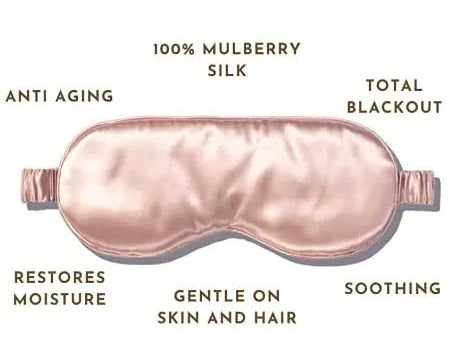
Sleep bra essentials: Sleep bras become your new nighttime uniform. Your surgeon might recommend 24/7 bra wearing for the initial weeks to provide consistent support during the critical healing period. Look for front-closure bras for ease of use, wireless or soft-cup bras to minimize pressure, and breathable materials for overnight wear.

The Complete Sleep Again Pillow System: Professional-Grade Lumpectomy Recovery
For patients who want to eliminate the trial-and-error of DIY pillow arrangements, the Sleep Again Pillow System addresses every positioning challenge discussed in this guide through integrated design and medical-grade materials.
Every Sleep Again Pillow System includes:
-
Two Contoured Side Pillows to cradle back and hips
-
Upper Body Wedge to create optimal upper body incline
-
Leg Support Wedge to gently elevate legs
-
Head Pillow to provide head support and neck mobility
-
Removable, washable slipcovers for every piece
Sleep Again Pillow System:
-
Everything you need: $299
-
Long-term value: Continues working for recovery, improved sleep, and future needs beyond lumpectomy
-
The real difference: Instead of hoping random pillows work together, you get a system engineered specifically for lumpectomy recovery that adapts as your healing progresses.
With that said, the Sleep Again Pillow System is the only full-body pillow system designed specifically for lumpectomy support.
Why Sleep Again Pillows Excel for Lumpectomy Recovery
Consistent therapeutic elevation: The Upper Body Wedge maintains the precise 30-40 degree angle that optimizes circulation and reduces swelling throughout the night. Unlike household pillows that compress and lose their therapeutic positioning, Sleep Again Pillows retain their shape when you need support most.
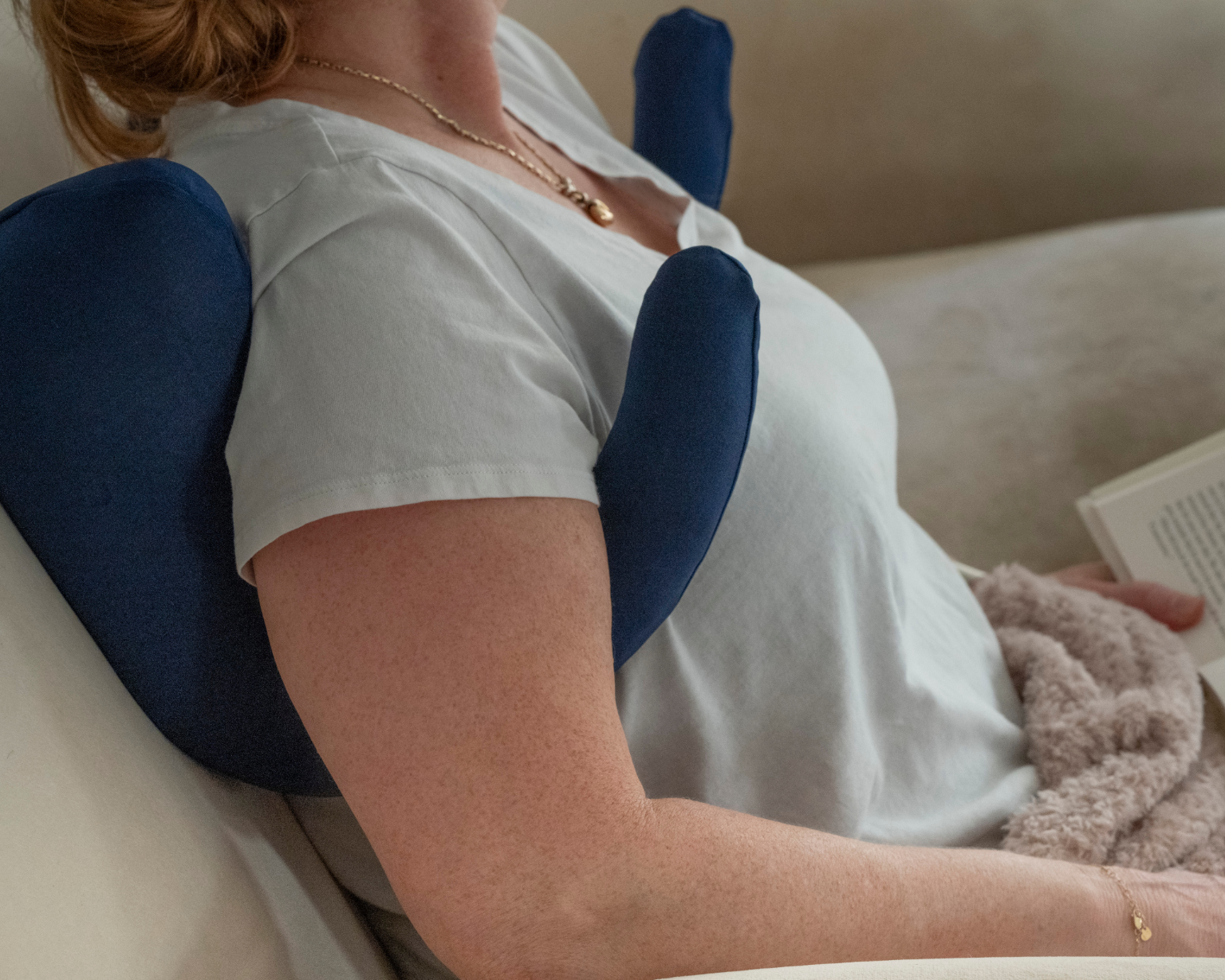
Surgical site protection: The Contoured Side Pillows create natural barriers that prevent unconscious rolling onto your surgical side while remaining comfortable to sleep against if you do shift during the night.
Comprehensive support system: Rather than hoping random pillows work together, each component is engineered to complement the others, creating seamless full-body support that adapts as your recovery progresses.
Hygiene advantage: The removable, washable covers address the cleanliness concerns crucial during recovery when you're spending more time in bed and may be dealing with drainage or medication-related needs.
Sleep Again Pillows vs. DIY Pillow Solutions: The Real Comparison
Setup time:
-
DIY pillow arrangement: 15-20 minutes nightly arranging and testing stability
-
Sleep Again Pillow System: 3-5 minutes once familiar with setup
Night maintenance:
-
DIY approach: 2-4 wake-ups for pillow readjustment when pillows compress and shift
-
Sleep Again Pillow System: Maintains positioning throughout sleep
Cost analysis:
-
DIY accumulation: $150-250 over multiple trial-and-error purchases
-
Sleep Again Pillows comprehensive solution: One integrated system designed specifically for lumpectomy recovery
SHOP THE BEST PILLOW FOR LUMPECTOMY RECOVERY

Recovery Timeline and Pain Management
Week 1: Focus on healing and protection with elevated back sleeping at 40-45 degrees. Take prescribed pain medication 30-45 minutes before bedtime and apply ice therapy as directed by your surgeon.
Week 2: Maintain protection while beginning gentle mobility. Reduce elevation to 30-35 degrees and introduce careful non-surgical side sleeping.
Week 3-4: Gradual return to varied positioning while monitoring comfort. Continue elevated back as primary position and increase side sleeping duration based on comfort.
Week 4+: Transition to sustainable long-term sleep habits with surgeon approval for position advances.
Sleep Troubleshooting Guide: Quick Fixes for Common Problems
Problem: "I’m worried about sliding down when I sleep."
Sleep Again Solution: Be sure to check out our Set Up Videos for flawless setup and sleep.
Problem: "My non-surgical arm keeps going numb."
Sleep Again Solution: Our system width is designed for full arm support
Problem: "I wake up rolled onto my surgical side."
Sleep Again Solution: Contoured Side Pillows act as natural, comfortable barriers
Problem: "My partner can't sleep with all these pillows."
Sleep Again Solution: Our modular system uses fewer pieces than DIY approaches and takes up an equal half of a standard Queen bed.
Frequently Asked Questions
Q: How long will I need to sleep in an elevated position after my lumpectomy?
A: Most surgeons recommend elevated back sleeping for several weeks, though this varies based on your specific surgery and healing progress. The first 1-2 weeks are typically the most critical for maintaining elevation.
Q: Can I sleep on my non-surgical side immediately after surgery?
A: Your non-operated side often becomes safe territory relatively quickly, but you should always check with your surgeon first. Even when cleared for side sleeping, proper support is essential to prevent unconscious rolling onto your surgical side during sleep.
Q: Why does my shoulder hurt more than my incision site?
A: Shoulder pain after lumpectomy often results from compensatory positioning and muscle tension as your body tries to protect the surgical site. Proper support and gentle movement can help alleviate this discomfort.
Q: When can I stop wearing a bra to sleep?
A: This depends on your surgery extent and surgeon's recommendations. Smaller procedures might only require a few days of bra support, while more extensive surgeries may require weeks of continuous support for optimal healing.
Q: Are expensive positioning pillows really worth it for a temporary recovery?
A: Quality positioning systems like the Sleep Again Pillow System often pay for themselves in improved sleep quality during the crucial first weeks of healing. Many patients continue using the system long after recovery for improved overall sleep quality.
Q: What if I accidentally roll onto my surgical side during sleep?
A: Occasional brief contact usually isn't harmful, but persistent pressure can interfere with healing. Use pillow barriers and consider positioning systems that prevent unconscious rolling.
Red Flags: When to Call Your Healthcare Team
While some discomfort is normal during lumpectomy recovery, certain symptoms warrant immediate medical attention:
Call your surgeon immediately for:
-
Signs of infection (increased redness, warmth, swelling, or unusual discharge from incision)
-
Sudden increase in pain that doesn't respond to prescribed medication
-
Fever over 101°F (38.3°C)
-
Persistent nausea or vomiting that prevents eating or drinking
Discuss with your healthcare provider:
-
Sleep problems that significantly worsen after the first week
-
Persistent numbness or tingling in your arm or hand
-
Questions about when to advance to different sleep positions
The Bottom Line: Your Recovery Sleep Success Plan
Lumpectomy recovery sleep challenges are real, but they're also temporary and manageable with the right approach. The key is understanding that elevated back sleeping isn't just a suggestion—it's a therapeutic intervention that directly supports your healing process.
Whether you choose a DIY approach with carefully selected pillows or invest in a comprehensive system like the Sleep Again Pillow System, the goal is to create sustainable comfort that works night after night. Your body is doing incredible healing work, and it deserves the best possible conditions for recovery.
Most importantly, be patient with yourself during this process. Recovery isn't linear, and some nights will be better than others. What matters is providing consistent, quality support that allows your body to heal while you rest.
Remember: good sleep isn't a luxury during recovery—it's a medical necessity that directly affects how quickly and completely you heal. You will sleep normally again. This recovery phase is temporary, even when it feels endless at 3 AM.
Medical Disclaimer
This information is provided for educational purposes only and should not replace professional medical advice. Every lumpectomy procedure and recovery process is unique, and sleeping position recommendations may vary based on your specific surgical approach, individual health conditions, and post-operative circumstances.
Always follow your surgeon's specific post-operative instructions regarding sleep positioning, activity restrictions, and recovery protocols. These medical guidelines take precedence over any general positioning advice provided here.
Contact your healthcare provider immediately if you experience concerning symptoms such as signs of infection, severe pain, persistent nausea, difficulty breathing, or any symptoms that worsen rather than improve during your recovery period.