You've decided to refresh your appearance with blepharoplasty, and you're researching recovery before surgery day. While your surgeon focuses on explaining incision techniques and healing timelines, one recovery factor rarely gets adequate attention: how you'll actually sleep for the next several weeks.
The position you sleep in after eyelid surgery isn't just about comfort—it's a critical factor determining minimal swelling that resolves quickly versus prolonged puffiness that extends recovery. Your sleeping position for the first two weeks will have more impact on your aesthetic results than expensive serums or supplements.
If you're reading this before your blepharoplasty, you have a significant advantage over patients who figure out post-surgery sleep positioning while dealing with anesthesia effects and uncomfortable swelling. This guide covers everything about sleeping after eyelid surgery, with a specific focus on head elevation techniques that accelerate healing and optimize results.
Why Sleep Positioning After Blepharoplasty Isn't Optional
After eyelid surgery, your sleep position directly impacts how quickly you recover and how well you heal.
When you undergo blepharoplasty, your surgeon creates precise incisions around delicate eye tissues. These tissues respond to surgical trauma with inflammation and fluid accumulation. Where that fluid goes and how quickly it drains depends almost entirely on the position of your head relative to your heart.
Three critical reasons head elevation matters:
Minimized Swelling and Bruising: Elevating your head 30-45 degrees above your heart allows gravity to assist lymphatic drainage away from your surgical sites. Fluid naturally drains downward rather than pooling around your eyes, resulting in less dramatic swelling and faster resolution of bruising. Patients who maintain proper elevation typically see noticeable improvement in puffiness within the first 72 hours.
Reduced Surgical Stress: The delicate tissues around your eyes are under significant strain immediately after surgery. Lying flat increases blood flow to the area, creating unnecessary pressure on fresh incisions and sutures. Elevated positioning reduces this hemodynamic stress, allowing tissues to heal with less tension and lower risk of complications like hematoma formation.
Accelerated Healing Timeline: When swelling is controlled through proper positioning, your body can focus healing resources on tissue repair rather than managing excessive inflammation. This translates to shorter recovery periods, less discomfort, and faster return to normal activities. Many surgeons report that patients who maintain consistent head elevation during the first two weeks heal 3-5 days faster than those who don't.
The positioning you choose for those critical first nights after surgery sets the foundation for your entire recovery trajectory. Proper positioning leads to optimal healing and results on schedule. Poor positioning extends your recovery timeline and can prolong swelling.
The Pre-Surgery Sleep Planner: Why Reading This Now Gives You an Advantage
If you're researching blepharoplasty recovery before your surgery date, you're ahead of most patients. While others will figure out sleep positioning through trial and error after surgery, you have the opportunity to prepare your sleep environment while thinking clearly, putting you in a better position to protect your results and speed up your recovery.
The preparation advantage:
Testing Your Setup: Experiment with elevated back sleeping now while comfortable. Spend a few nights at 30-45 degrees using whatever support systems you're considering. This reveals what works before dealing with post-surgical discomfort.
Making Informed Equipment Decisions: Shopping for positioning equipment after surgery leads to impulsive purchases. Planning ahead allows you to research options and invest in equipment that supports quality sleep throughout recovery.
Environmental Preparation: Your bedroom needs modifications for optimal recovery. Clearing nightstand space, arranging appropriate lighting, and setting up easy access to supplies are simple when done in advance.

What Makes Elevated Back Sleeping the Gold Standard for Blepharoplasty Recovery
Among all sleeping positions after eyelid surgery, elevated back sleeping is the medically optimal choice. This isn't about comfort preference—it's about positioning that aligns with the physiological needs of healing eye tissues.
The 30-45 Degree Therapeutic Range:
This elevation range isn't arbitrary. At 30-45 degrees, your head is elevated enough to facilitate gravity-assisted fluid drainage while remaining comfortable for sustained sleep. Lower than 30 degrees loses drainage benefits; higher than 45 degrees creates neck strain and upper back tension that fragments sleep.
Why Back Sleeping Is Non-Negotiable:
Side sleeping after blepharoplasty creates asymmetric pressure on surgical sites and can lead to uneven swelling. The compression from pillow contact can stress fresh incisions and potentially compromise sutures. Stomach sleeping is completely off the table—direct facial pressure would be counterproductive to every healing goal.
Back sleeping in an elevated position accomplishes several therapeutic objectives:
Bilateral Symmetry: Both eyes receive identical positioning support, promoting even healing and reducing asymmetric swelling risk.
Cervical Spine Alignment: Proper elevated back sleeping maintains a neutral neck position, preventing the muscle tension and headaches that develop with inadequate pillow arrangements.
Respiratory Optimization: The semi-upright position keeps airways open and reduces sleep apnea tendencies, which can be exacerbated by facial swelling.
Sustained Comfort: Unlike improvised positions that shift throughout the night, proper elevated back sleeping can be maintained for full sleep cycles, allowing deep restorative sleep phases essential for healing.
Patients who achieve the fastest, most aesthetically pleasing results after blepharoplasty are those who commit to elevated back sleeping from night one and maintain it consistently through the critical first two weeks.

The Sleep Again Pillow System for Blepharoplasty Recovery
While some patients successfully manage post-blepharoplasty sleep positioning with household items, many find that investing in a dedicated recovery positioning system eliminates the trial-and-error frustration and provides consistent support that household solutions simply cannot match.
When DIY Positioning Falls Short:
Standard pillows present several limitations for post-surgical recovery. They compress throughout the night, losing the therapeutic elevation angle when you need it most. They shift position during normal sleep movements, requiring middle-of-the-night readjustments that fragment restorative sleep. They rarely provide the full-body support needed to maintain elevated positioning comfortably for 7-8 hours.
Patients who attempt DIY solutions often purchase multiple pillow sets, trying to find the right combination, ultimately spending as much or more than a professional system would cost. The frustration of waking up multiple times per night to readjust pillows during critical healing periods adds unnecessary stress to recovery.
The Sleep Again Pillow System Advantage:
The Sleep Again Pillow System is specifically engineered to maintain the therapeutic 30-45 degree elevation angle throughout the night without compression or shifting. The structured design provides comprehensive support from head to lower back, preventing neck strain and upper back discomfort that commonly develops with improvised pillow arrangements.
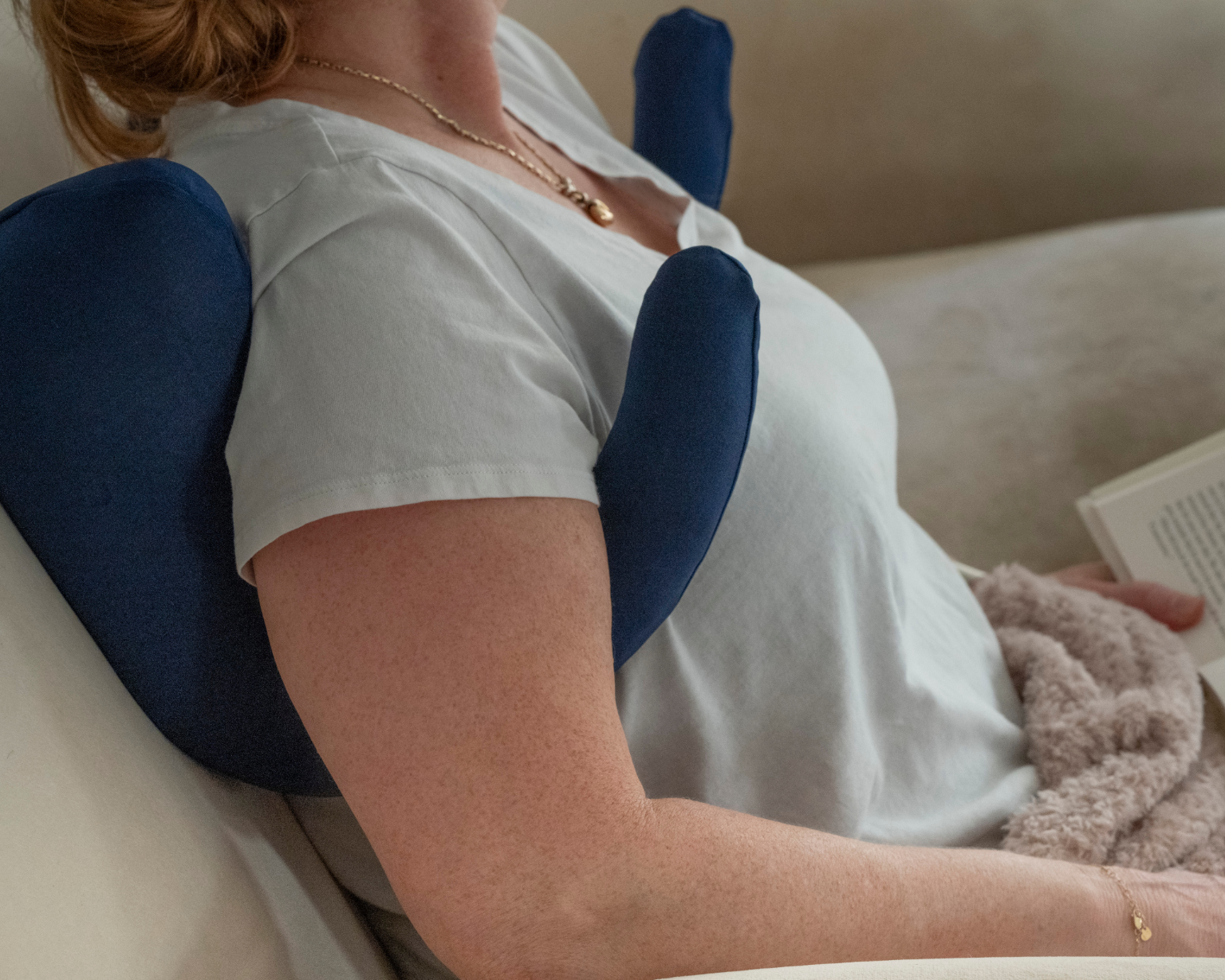
What's Included in the Sleep Again Pillow System:
Every Sleep Again Pillow System includes five integrated components designed to work together for optimal post-surgical positioning:
-
Two Contoured Side Pillows to cradle the back and hips
-
Upper Body Wedge to create optimal upper body incline
-
Leg Support Wedge to gently elevate legs
-
Head Pillow to provide head support and neck mobility
-
Removable, washable slipcovers for every piece
The integrated design ensures all components work together to maintain proper positioning. The contoured side pillows prevent unconscious rolling during sleep, while the upper body wedge maintains the precise therapeutic angle without compression. The leg support wedge reduces lower back strain that commonly develops during extended elevated positioning.
All components feature removable, washable slipcovers for hygiene during recovery when cleanliness is particularly important. This practical feature allows you to maintain fresh, clean bedding throughout your healing process without compromising your positioning setup.
Pre-Surgery Planning Consideration:
For patients who know they struggle with back sleeping or who have previous experience with DIY recovery positioning that proved frustrating, investing in a dedicated positioning system before surgery eliminates uncertainty. You can test the system, confirm it works for your body, and have it ready for immediate use when you return home from surgery—removing one significant variable from your early recovery experience.
Many patients find that having a reliable positioning system ready before surgery reduces pre-operative anxiety. Knowing your sleep setup is already solved allows you to focus mental energy on other aspects of surgical preparation and recovery planning. The ability to test the system in advance means you can make adjustments or exchanges if needed, rather than being committed to an uncomfortable solution during your healing period.
The investment in professional positioning equipment often pays for itself through shorter recovery times, better sleep quality during healing, and reduced need for additional recovery aids or remedies.
Common Sleep Positioning Mistakes That Extend Blepharoplasty Recovery
Understanding what not to do is as valuable as knowing the optimal approach. These mistakes are common among blepharoplasty patients, and each one can add days or weeks to your recovery timeline.
Stacked Pillow Failures:
Many patients attempt to create elevation by stacking standard bed pillows behind their back and head. This approach fails for predictable reasons. Standard pillows compress under body weight, gradually losing height throughout the night. Pillow stacks shift and scatter during normal sleep movements, requiring frequent readjustments that fragment restorative sleep.
Recliner Positioning Problems:
Sleeping in a recliner creates problems for blepharoplasty recovery. Recliners position your body in ways that create lower back strain, restrict leg circulation, and often place your head at angles too steep for comfortable, sustained sleep. The physical discomfort from the recliner itself can rival post-surgical discomfort after several nights.
Side Sleeping Attempts:
Some patients believe sleeping on the opposite side from their dominant surgical site is acceptable. This reasoning is incorrect because all blepharoplasty requires bilateral healing considerations. Even if one side needs more extensive work, both eyes benefit from symmetrical positioning. Side sleeping also makes it nearly impossible to maintain the therapeutic 30-45 degree elevation angle.
Unconscious Position Changes:
The most common mistake involves unconscious position changes during sleep. Patients fall asleep properly elevated but shift to their preferred sleep position during the night. This cycle of position loss creates anxiety and disrupts sleep quality. Professional positioning systems address this by making it physically difficult to shift out of therapeutic positions during sleep.
Recognizing these patterns now, while you're in the planning phase, allows you to choose positioning solutions that actively prevent these mistakes rather than requiring constant conscious effort to avoid them.
Week-by-Week Sleep Positioning Through Blepharoplasty Recovery
Your sleep positioning needs evolve as your healing progresses. Understanding these phases helps you adjust appropriately.
Week 1: The Critical Foundation
Strict 30-45 degree elevation is non-negotiable during the first seven days. Swelling peaks during days 2-4, making your positioning during this window crucial. Expect minimal sleep the first two nights as you adjust, but most patients adapt by nights 3-4. Consistency matters—even brief periods lying flat can undo hours of proper positioning.
Weeks 2-3: Maintaining Momentum
Continue elevated sleeping even as swelling reduces and you feel better. Internal healing lags visible improvement. Patients who abandon positioning too early often experience swelling rebound that extends recovery by several days.
Weeks 4+: Gradual Transition
Most surgeons allow lower elevation angles around week three or four. Reduce gradually, monitoring your body's response. Many patients maintain mild elevation long-term for ongoing cosmetic benefits.

Creating Your Optimal Blepharoplasty Sleep Environment
Your sleep environment impacts recovery comfort. Address these factors during pre-surgery planning:
Environmental Controls: Cool room temperatures (65-68°F) reduce inflammation. Install blackout curtains for light sensitivity. Set the humidity to 40-50% to prevent eye dryness. Position fans to avoid direct facial airflow.
Bedside Organization: Arrange within reach: eye drops, ointments, pain medications, water, tissues, gauze pads, a small mirror, and your phone with your surgeon's number programmed. Set up everything before surgery.
Medical Considerations Beyond Positioning
Medication Timing Strategy:
Work with your surgeon to optimize pain medication timing around your sleep schedule. Taking medications 30-45 minutes before bed allows them to reach peak effectiveness as you're falling asleep.
Eye Care Protocol:
Your surgeon will prescribe eye drops, ointments, or cold compresses for recovery. Establish a bedtime eye care routine and keep supplies accessible. Apply ointments or drops just before settling into your sleeping position.
Swelling Assessment:
Monitor morning versus evening swelling patterns. If you notice significantly more puffiness in the morning despite proper elevation, discuss this with your surgeon.
Activity Restrictions:
Follow your surgeon's guidelines about when you can resume exercise, bend over, or lift objects. Violations of these restrictions can undo the benefits of proper sleep positioning.
Nutritional Support:
Some studies suggest that most patients are nutrient-depleted before and after surgery. Before + After Vitals, a supplement specifically designed for cosmetic surgery recovery, can help enhance recovery and improve results after surgery.
When to Contact Your Surgeon About Sleep-Related Concerns
While most blepharoplasty recovery proceeds smoothly, certain symptoms warrant immediate medical attention: severe asymmetric swelling (especially with increasing pain), vision changes beyond temporary blurriness from ointments, intensifying pain after the first 48 hours, significant breathing difficulties in elevated position, or pressure sores from positioning equipment. Trust your instincts—if something feels wrong, contact your surgeon.
FAQs About Sleeping After Blepharoplasty
How long do I need to sleep elevated after eyelid surgery?
Most surgeons recommend a strict 30-45 degree elevation for the first two weeks, with a gradual transition during weeks 3-4. Individual healing varies—follow your surgeon's specific timeline. Many patients maintain mild elevation even after restrictions lift due to cosmetic benefits.
Can I sleep on my side at all during blepharoplasty recovery?
No side sleeping during the first 2-3 weeks. Side positioning creates asymmetric pressure and uneven swelling. Both eyes need symmetrical healing conditions, even if one side had more extensive work. After week three, gradual side sleeping may be possible with surgeon approval.
What happens if I accidentally roll over in my sleep?
Brief position changes typically don't cause major issues if you return to proper positioning quickly. Extended periods (multiple hours) in the wrong positions can increase swelling and stress on incisions. The Sleep Again Pillow System and its two side support pillows prevent rolling onto the side during the night.
Will sleeping elevated help reduce bruising?
Yes, significantly. The 30-45 degree angle facilitates drainage, helping your body process blood that causes discoloration. Patients maintaining consistent elevation typically see bruising fade 3-5 days faster. However, some bruising is inevitable—elevation minimizes rather than eliminates it.
Can I use regular bed pillows, or do I need special equipment?
Regular pillows can work but have limitations: they compress overnight, shift during sleep movements, and rarely provide adequate back/neck support for 7-8 hours without muscle strain.
Is sleeping in a recliner better for blepharoplasty recovery?
No. Recliners typically exceed therapeutic 30-45 degrees, causing neck strain. They restrict leg positioning, impairing circulation and causing discomfort. Physical strain from recliner sleeping often rivals post-surgical discomfort. Proper positioning systems in your bed are superior.
When can I return to stomach sleeping?
Avoid stomach sleeping for at least 3-4 weeks, with many surgeons recommending 6 weeks. Stomach sleeping creates direct facial pressure that can compromise incisions and affect results. When you do resume, do so gradually and monitor for morning puffiness increases.
Does elevated sleeping help prevent infection?
Indirectly, yes. Elevation reduces inflammation, promotes circulation, and supports immune function at surgical sites. Elevated positions also reduce eye rubbing during sleep, minimizing bacteria introduction to incisions. However, elevation doesn't replace proper hygiene and antibiotic compliance.
Can I take sleep medications after surgery?
Discuss with your surgeon beforehand. Some sleep aids interact poorly with pain medications or increase fall risk. If appropriate, your surgeon may recommend specific types. Many patients find that optimizing positioning eliminates sleep aid needs.
How do I know if my elevation angle is correct?
The 30-45 degree angle roughly corresponds to comfortably reading a book without it sliding off your chest. Nearly upright means too steep (causing neck discomfort). Only slightly elevated means insufficient therapeutic benefit. Use smartphone protractor apps to measure before surgery.
Should I maintain elevation for daytime naps?
Yes, all sleep periods during the first two weeks need 30-45 degree elevation, including naps. Brief rest in a regular chair is fine, but actual sleep requires elevated positioning. Benefits are cumulative—even a 20-minute flat nap can undo hours of proper positioning.
Important Medical Disclaimer
The information provided on this page is for educational purposes only and should not replace professional medical advice from your healthcare provider. Sleep Again Pillows are positioning support products designed to help maintain sleep positions recommended by medical professionals during recovery and for therapeutic use.
Always follow your surgeon's or physician's specific post-operative instructions and positioning requirements. Medical guidance from your healthcare team takes precedence over any general information provided here. Recovery timelines, positioning angles, and product suitability vary based on individual surgical procedures, medical conditions, and patient-specific factors.
Consult your healthcare provider before purchasing positioning equipment if you have specific medical concerns or questions about whether these products are appropriate for your recovery or medical condition(s). Your medical team can provide personalized recommendations based on your unique situation.
Sleep Again Pillows do not diagnose, treat, cure, or prevent any medical condition. These products provide positioning support to help maintain sleep angles and positions as directed by your healthcare provider.