Most lumpectomy patients spend weeks researching the surgery itself. Far fewer think about what happens when the lights go out.
Sleep position during recovery is one of those details that feels minor until you're three days post-op, exhausted, and trying to figure out how to get comfortable. The truth is, how you sleep after lumpectomy directly affects wound healing, swelling, and your long-term results — and knowing what to expect before surgery makes an enormous difference.
Understanding Post-Lumpectomy Sleep Position Requirements
A lumpectomy removes cancerous or abnormal tissue while preserving healthy breast tissue. The procedure is less invasive than a mastectomy, but your body still needs protected healing time.
Most surgeons require back sleeping for one to four weeks after lumpectomy. The specific timeline depends on incision location, whether lymph nodes are removed, and whether surgical drains are placed. Your surgeon will provide exact guidelines based on your case.
CHECK OUT OUR GUIDE ON BACK SLEEPING AFTER A LUMPECTOMY
Back sleeping during initial recovery serves several critical functions:
-
Prevents pressure on healing incisions and reduces wound complication risk
-
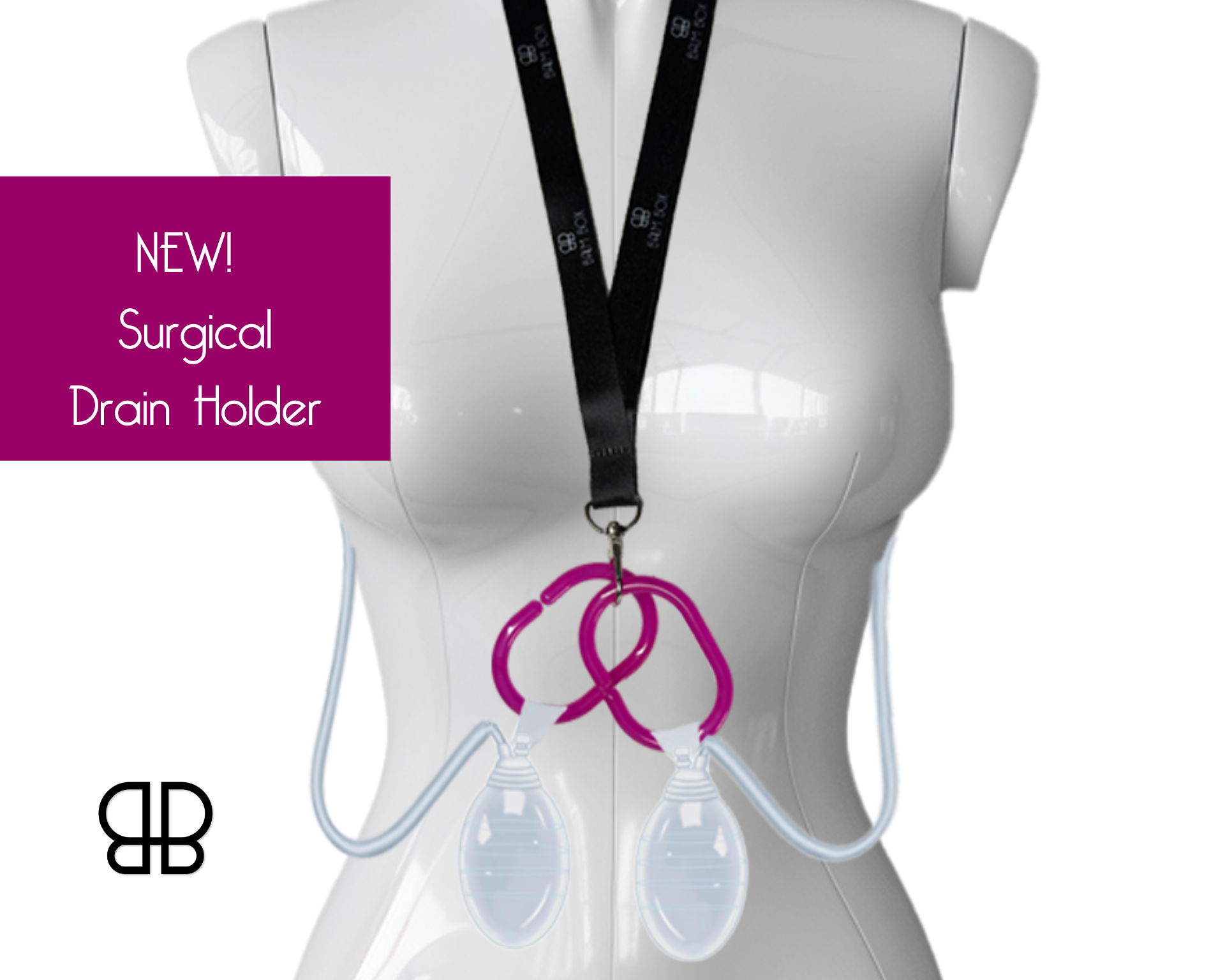
Maintains proper positioning for surgical drains if placed
-
Minimizes pain and swelling in breast tissue
-
Supports optimal healing and aesthetic outcomes
The transition back to side sleeping happens gradually after your surgeon provides clearance, and it's critical that you follow their guidelines over anything you read online.
Planning for this transition before surgery means you'll have the right support in place when you need it.
What Happens During the Side Sleeping Transition
Once cleared for side sleeping, your breast tissue will still be tender and sensitive. Internal healing continues for weeks after surgery. The area where tissue was removed needs time to fully recover, and you may experience numbness, tingling, or hypersensitivity from nerve healing.
Side sleeping creates new sensations. Gravity pulls breast tissue differently than when sleeping on one's back. Your arm rests against your chest in ways that may feel uncomfortable initially. Many patients report feelings of being "unsupported" or experiencing pulling sensations near the incision site.
The good news: this discomfort is temporary and manageable with proper support. Most people return to comfortable side sleeping within four to six weeks of surgery when they use appropriate positioning aids to help support the breast while healing.

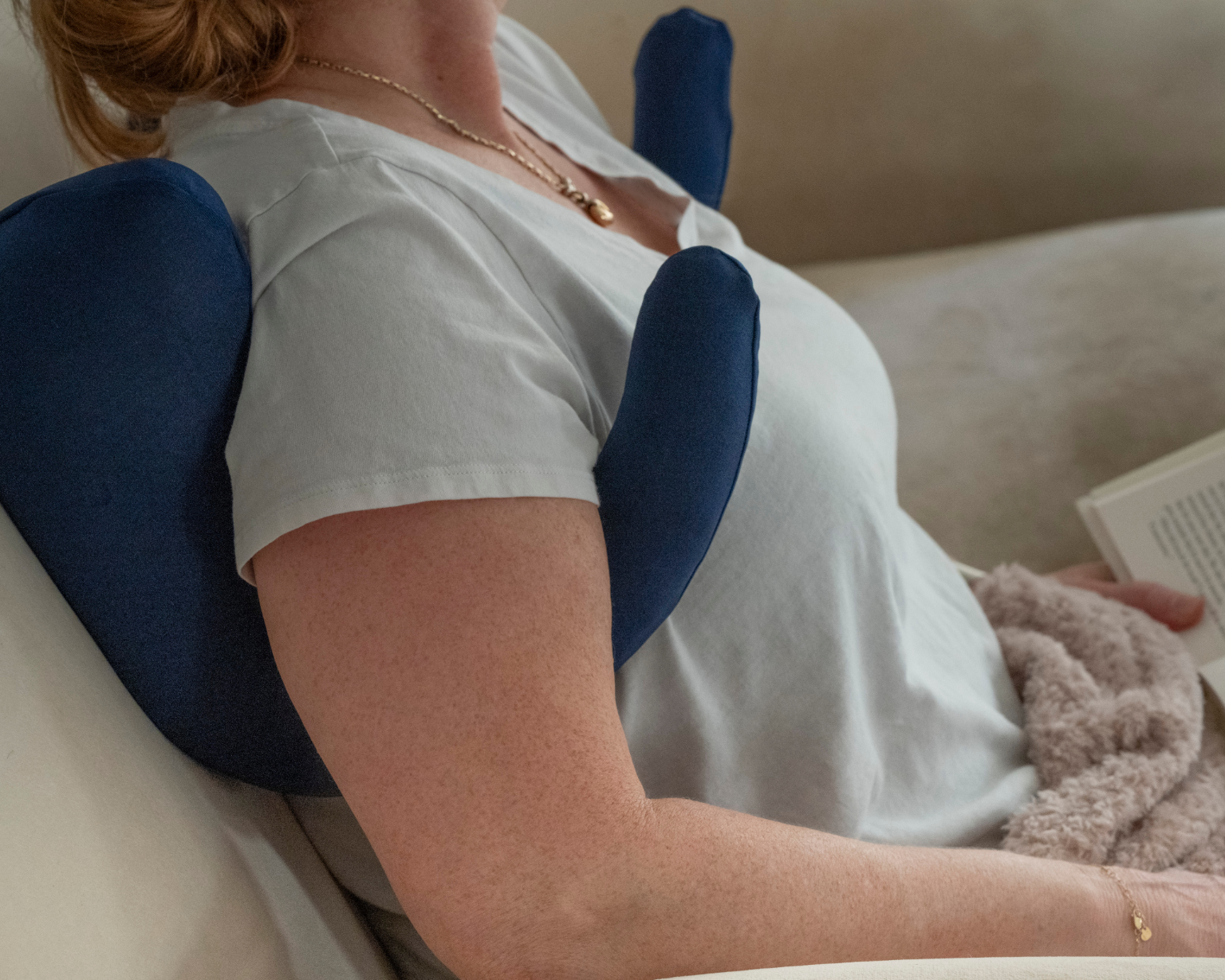
The Side Sleeping Chest Pillow: Purpose-Built Recovery Support
After experiencing multiple breast surgeries, we created the Side Sleeping Chest Pillow to address the specific mechanical challenge of post-surgical side sleeping.
The design solves problems standard pillows can't:
Adjustable width positioning. Customize the pillow's sides to perfectly cradle your chest while providing back support. As recovery progresses and swelling decreases, adjust the width to match changing comfort needs.
Symmetrical design for natural movement. Turn freely from right side to left side throughout the night without losing support or needing to readjust positioning.
Dual-function support system. Unlike standard pillows, the design provides both chest cradling and back support simultaneously—the exact combination post-surgical patients need during the transition period.
The Side Sleeping Chest Pillow addresses the specific challenges of transitioning from back sleeping to side sleeping after lumpectomy, mastectomy, or breast reconstruction. It ships quickly from the USA and Canada, so you can order before surgery and have it ready for the transition phase.
Important note: Due to federal regulations, bedding products aren't returnable, and all sales are final. This pillow was designed based on what we needed during our own recoveries and has become a trusted tool for thousands of breast surgery patients.
SHOP THE SIDE SLEEPING CHEST PILLOW
The Timeline: What to Expect Week by Week
Weeks 1-2: Strict back sleeping. Your incisions are healing, internal stitches are dissolving, and breast tissue is recovering from surgical trauma. No side sleeping during this phase.
Weeks 2-4: Continue back sleeping unless your surgeon provides specific clearance. Some patients with straightforward procedures may begin transitioning during week three. Others need the full four weeks or longer.
Weeks 4-6: Most patients receive clearance to attempt side sleeping during this window. Start with short sessions while awake before committing to full nights of side sleeping.
Beyond 6 weeks: Gradual return to normal sleep positions, though some patients need additional time before stomach sleeping feels comfortable.
Your surgeon's timeline supersedes these general guidelines. Factors such as incision healing, drain removal, and individual recovery progression determine your specific clearance.

Why Standard Pillows Don't Provide Adequate Post-Surgical Support
Regular bed pillows were designed for head support, not post-surgical chest stabilization. They're too soft to maintain consistent positioning, too thick to adjust to specific needs, and they flatten or shift throughout the night.
Standard pillows create several problems during lumpectomy recovery:
The support isn't targeted. Hugging a pillow to your chest provides some cushioning but doesn't address the dual need for chest cradling and simultaneous back support.
The positioning isn't stable. Regular pillows require constant readjustment, which disrupts sleep and potentially strains healing tissue.
The design doesn't accommodate movement. Building multiple-pillow arrangements works until you naturally shift positions during sleep, which everyone does regardless of sleeping style.
SHOP THE SIDE SLEEPING CHEST PILLOW
Preparing Your Sleep Environment Before Surgery
Setting up optimal sleep conditions before your procedure means less stress during recovery.
Temperature control. Many patients experience night sweats or temperature sensitivity after surgery, particularly if hormonal changes from cancer treatment are involved. Set your bedroom thermostat to 65-68 degrees Fahrenheit. Invest in breathable, natural-fiber sheets. Have extra blankets accessible for easy temperature adjustment.
Elevation options. Even after side sleeping clearance, keeping your upper body slightly elevated reduces swelling and improves comfort. The Side Sleeping Chest Pillow works effectively with wedge pillows or adjustable beds. The combination provides specialized chest support for side sleeping plus elevation that promotes lymphatic drainage and reduces pressure on healing tissue.
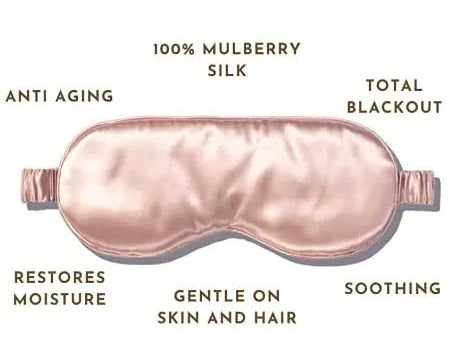
Lighting management. Your body heals during sleep, so quality matters significantly. Install blackout curtains or purchase a sleep mask. Remove electronic devices from the bedroom. Establish pre-sleep routines that signal your body it's time to rest.
Partner communication. If you share a bed, discuss physical space needs, which side your partner should use to avoid the surgical side, and whether a body pillow between you provides a protective buffer. Some couples use separate beds temporarily during initial recovery. Address these logistics before surgery rather than navigating them while recovering.
Managing Discomfort During the Transition
Even with proper support, some discomfort occurs during the transition to side sleeping.
Pain medication timing. If your doctor prescribes pain medication or recommends over-the-counter options, taking it 30-45 minutes before bed helps you settle into sleep more comfortably.
Pre-bed ice application. Apply a soft ice pack (wrapped in a thin towel) to your breast for 15-20 minutes before bed to reduce inflammation and discomfort. Don't sleep with ice on your chest—avoid extended cold exposure that could damage skin.
Knee positioning. Placing pillows between your knees takes pressure off your lower back and hips, making it easier to maintain comfortable side sleeping without unconsciously shifting in ways that might disturb your chest. Combined with chest support from the Side Sleeping Chest Pillow, this creates full-body alignment that reduces compensatory tension. Your body doesn't work to maintain position, which means less energy is spent on positioning and more energy is available for healing.
Breathing techniques. Tension and anxiety about discomfort can increase pain perception. Spend five minutes doing slow, deep breathing before bed—inhale for four counts, hold for four, exhale for four. This activates your parasympathetic nervous system and reduces both physical tension and pain sensitivity.
Warning Signs That Require Medical Attention
Most discomfort during the transition to side sleeping is a normal healing sensation.
Certain signs warrant immediate contact with your surgeon:
-
Sharp, increasing pain that doesn't improve with position changes
-
Visible swelling that develops after sleeping on your side
-
Warmth, redness, or unusual discharge from your incision
-
Sensation that your incision is pulling apart or opening
-
Fever or chills accompanying sleep position discomfort
Trust your instincts. If something feels wrong, contact your medical team.
Sleep Position and Long-Term Surgical Outcomes
Sleep position during recovery influences long-term results. Back sleeping during the initial lumpectomy healing allows breast tissue to settle and heal in a neutral position. This affects the final appearance of your breast, particularly if tissue was rearranged or repositioned during lumpectomy.
Gradual transition to side sleeping helps tissue adapt to different positions without trauma. Rushing this process or sleeping without proper support can lead to:
-
Asymmetrical healing if you favor one side over the other
-
Increased scar tissue formation from repeated tension on healing areas
-
Prolonged swelling due to poor lymphatic drainage
-
Sleep debt that compromises immune system function and healing capacity
Your sleep position is part of your treatment plan, not just a comfort preference.
FAQs: Side Sleeping After Lumpectomy
How long will I need to sleep on my back after a lumpectomy?
The typical timeline ranges from one to four weeks, depending on your case complexity and healing progression. Your surgeon will assess incision integrity and tissue recovery before providing clearance for side sleeping. Individual factors significantly impact this timeline, which is why your surgeon's specific guidance is essential.
Can I sleep on the side that didn't have surgery right away?
Not necessarily. Even though only one breast had surgery, sleeping on your unaffected side can still put pressure on your chest and potentially affect healing. Your surgeon will advise when it's safe to try sleeping on either side.
Will I ever be able to sleep on my stomach again after a lumpectomy?
Many patients eventually return to stomach sleeping, but this typically takes longer than side sleeping—usually 6-12 weeks or more. Breast tissue needs full recovery before tolerating the direct pressure of stomach sleeping. Discuss your specific timeline with your surgeon.
How will I know when I'm ready to transition from back sleeping to side sleeping?
Your surgeon provides clinical clearance based on incision healing and recovery progress. Beyond that, readiness indicators include: lifting your arm on the affected side without sharp pain, wearing a regular bra comfortably (if that's part of your recovery plan), and touching your breast without significant tenderness. If these symptoms persist, your body needs more back sleeping time.
Does sleeping position affect radiation therapy if I need it after a lumpectomy?
Radiation therapy often begins several weeks after lumpectomy surgery. Your radiation oncologist may have specific sleep position recommendations to help manage skin sensitivity during treatment. Coordinate with both your surgeon and radiation oncologist about optimal sleep approaches during this phase.
Can I use a weighted blanket after a lumpectomy?
Wait for surgical clearance before using weighted blankets. The added pressure, even though distributed across your body, can affect healing tissue and drainage. Once you're healed enough for side sleeping, you can gradually reintroduce a weighted blanket if desired.
How soon can I sleep without a surgical bra or compression garment?
This varies significantly based on your surgeon's preferences and procedure specifics. Some surgeons recommend wearing supportive garments for 2-4 weeks, while others have different timelines. Never discontinue prescribed compression garments without surgeon approval, even if uncomfortable sleeping in them.
Should I order the Side Sleeping Chest Pillow before or after surgery?
Order before surgery so it's ready when you reach the transition phase. Having proper support available eliminates the need to shop while recovering and ensures you're fully prepared.
How does side sleeping affect drain care if I have surgical drains?
With drains in place, you'll need to maintain back sleeping until they're removed. Once drains come out, you'll still need surgical clearance before attempting side sleeping, though the timeline often becomes more flexible at that point.
Why does sleep quality matter so much during lumpectomy recovery?
Your body performs critical healing work during deep sleep stages. During these phases, your body releases growth hormone, which repairs tissue damage and builds new cells. Quality sleep also regulates inflammation, supports immune function, and helps manage pain sensitivity. Poor sleep can slow wound healing and increase discomfort perception. Creating optimal sleep conditions—including proper positioning—isn't just about comfort; it's a genuine recovery strategy that influences how quickly and completely you heal.
What makes the Side Sleeping Chest Pillow different from regular pillows for recovery?
Standard pillows address one need (head support), but post-surgical side sleeping requires solving two simultaneous problems: preventing chest pressure while maintaining body alignment. The Side Sleeping Chest Pillow was created by a breast cancer survivor specifically for this transition phase, not adapted from a general-purpose design. It maintains support through natural sleep movement rather than requiring constant readjustment, which means better sleep quality when your body needs it most for healing.
What other items should I prepare before surgery for optimal sleep recovery?
Beyond the Side Sleeping Chest Pillow, several items improve post-surgical sleep comfort. If your doctor prescribes elevated back sleeping for more than two weeks following your lumpectomy, the Sleep Again Pillow System is the only full-body pillow system designed specifically to support elevated back sleeping after surgery. Both are FSA and HSA eligible.
When is the best time to order recovery support items?
Order your recovery items at least two to three weeks before your scheduled surgery date. The last thing you want is waiting for deliveries while recovering or asking someone else to handle these preparations. Having your sleep setup ready before surgery eliminates stress and lets you focus entirely on healing.
Preparing Now for Smoother Recovery
Lumpectomy recovery involves more than healing incisions—it's about giving your whole body what it needs to recover, and sleep is a cornerstone of that process.
The transition from back sleeping to side sleeping represents your body returning to normal. Being able to sleep in your preferred position again is a tangible sign of healing, and having the right support makes that transition safer and more comfortable.
Planning ahead reduces stress during recovery. Some recovery phases will be more comfortable than others. You might be ready for side sleeping earlier than expected, or you might need more time than initially anticipated. Both outcomes are normal.
The important thing is supporting your body's healing process with proper positioning, adequate rest, and patience.
Disclaimer
The information provided on this page is for educational purposes only and should not replace professional medical advice from your healthcare provider. Sleep Again Pillows are positioning support products designed to help maintain sleep positions recommended by medical professionals during recovery and for therapeutic use.
Always follow your surgeon's or physician's specific post-operative instructions and positioning requirements. Medical guidance from your healthcare team takes precedence over any general information provided here. Recovery timelines, positioning angles, and product suitability vary based on individual surgical procedures, medical conditions, and patient-specific factors.
Consult your healthcare provider before purchasing positioning equipment if you have specific medical concerns or questions about whether these products are appropriate for your recovery or medical condition(s). Your medical team can provide personalized recommendations based on your unique situation.
Sleep Again Pillows do not diagnose, treat, cure, or prevent any medical condition. These products provide positioning support to help maintain sleep angles and positions as directed by your healthcare provider.