Your appendix has been causing trouble, and surgery is on the schedule. You've probably already mapped out the logistics — who's driving you home, how much time off work, what soft foods to stock in the fridge. But here's the thing most people forget to plan for until they're home from the hospital, uncomfortable and completely stumped: how are you actually going to sleep?
Post-appendectomy sleep is one of the most overlooked parts of recovery planning — and one of the most important. The position you sleep in directly affects healing speed, gas-related discomfort, incision protection, and sleep quality. Get it right before your surgery date, and recovery becomes significantly more manageable.
This guide is written for the proactive patient: someone who wants to walk into surgery knowing exactly what their sleep setup will look like on the other side. By the end, you'll have everything you need, including knowing why elevated back sleeping is the clinical gold standard after an appendectomy, how to build a sleep environment that supports it, and which tools — including purpose-built recovery positioning systems — are worth having in place before you ever leave the hospital.
What Is an Appendectomy and Why Does It Affect Sleep?
An appendectomy is the surgical removal of the appendix — a small, finger-shaped pouch attached to the large intestine in the lower right abdomen. The procedure is performed to treat appendicitis, an inflammation of the appendix that, left untreated, can progress to rupture and serious complications.
Most appendectomies today are performed laparoscopically: the surgeon makes one to three small incisions near the navel, inflates the abdomen with carbon dioxide (CO₂) gas to create working space, and removes the appendix through those small portals. Open appendectomy — a single larger incision — is used in more complex cases, including ruptured appendix situations. Recovery timelines differ between the two, but sleep positioning principles remain largely the same.
Here's why sleep becomes complicated after either approach:
Abdominal muscle disruption. The core muscles your body relies on to roll over, sit up, and shift positions in bed have been manipulated during surgery. They're sore, swollen, and temporarily weakened.
CO₂ gas accumulation. For laparoscopic procedures, the inflation gas doesn't fully exit before you go home. Trapped gas migrates upward and causes referred pain in the shoulders and chest — a puzzling symptom that's entirely normal but strongly influenced by sleep position.
Incision sensitivity. Even small laparoscopic ports leave tender incision sites. Pressure, twisting, or stretching across those areas adds unnecessary pain to an already uncomfortable recovery.
Post-anesthetic sleep disruption. General anesthesia temporarily disrupts normal sleep architecture. Quality positioning helps compensate by maximizing physical comfort during rest.
The good news: all of these challenges are addressable with the right sleep strategy — and you can have that strategy ready to deploy the moment you get home.
Why Is Elevated Back Sleeping the Gold Standard After Appendectomy?
Ask any surgeon what position their appendectomy patients should sleep in, and "back sleeping with elevation" will be the consistent answer. This isn't just convention. There's a solid biomechanical logic behind it.
What does "elevated" actually mean? The target range is 30 to 45 degrees of upper body incline. Think of a reclined position — not fully flat, not bolt upright. This angle does several important things simultaneously.
How Does Elevation Reduce CO₂ Gas Pain?
The CO₂ used to inflate the abdomen during laparoscopic surgery needs to be reabsorbed and expelled over the hours and days post-procedure. Lying flat allows gas to pool against the diaphragm, producing the aching referred pain in the shoulder and chest that surprises so many post-laparoscopic patients. At a 30–45 degree incline, gravity encourages gas to move away from the diaphragm toward areas of the body better equipped to process and eliminate it — significantly reducing discomfort and speeding resolution of gas-related symptoms.
How Does Back Sleeping Protect the Incision Site?
Sleeping on your back keeps your abdominal wall in a neutral, unstressed position. There's no twisting, no lateral pressure, and no body weight pressing down on incision sites the way it would if you were on your side.
At 30–45 degrees, your torso maintains a gentle bend that keeps abdominal muscles in a relaxed, shortened state, eliminating the stretching tension across healing tissue that flat sleeping creates. This same elevated position also distributes body weight over a larger surface area, reduces pressure points, and supports circulation to deliver oxygen and nutrients to healing tissue more efficiently.
What Are the Sleep Positions to Avoid After an Appendectomy?
Understanding what not to do is just as important as knowing the ideal position.
Why can't I sleep on my stomach after an appendectomy?
Stomach sleeping is the position to avoid most firmly during recovery. When you sleep face-down, your entire body weight compresses directly onto the abdominal region — exactly where your surgical site, healing tissue, and any residual gas happen to be. This creates concentrated pressure on incision sites, forces abdominal muscles into a stretched position, and significantly increases pain.
When can I sleep on my side after an appendectomy?
Most patients can cautiously reintroduce side sleeping after the first 7–10 days with their surgeon's guidance. The right side — where the appendix was located, and incisions sit — puts direct lateral pressure on the surgical area and should be avoided longest. The left side is generally better tolerated but still requires a pillow between the knees to maintain hip alignment and reduce abdominal muscle tension. The bigger early-recovery risk with side sleeping is unconscious rolling: if abdominal muscles haven't regained stability, an involuntary shift during sleep can wake you with significant pain. Properly supported back sleeping eliminates that risk entirely.
What about sleeping in a recliner?
Many appendectomy patients instinctively migrate to a recliner in the first few nights post-surgery, and there's a real logic to it: recliners naturally provide the 30–45 degree incline that's therapeutically beneficial, and they limit unconscious rolling.
But here's the thing. A recliner may be a reasonable short-term bridge, but it's not a substitute for a properly supported bed-based setup built around the same therapeutic angles. Plus, if you don't already own a recliner, renting a medical recliner can be expensive and hard to maneuver.
How Do You Get In and Out of Bed After an Appendectomy?
Getting into and out of bed is one of the most overlooked pre-surgery skills, and one of the most immediately relevant once you're home. The standard sit-up approach engages your abdominal muscles directly and will be genuinely painful in the first week post-op. The log-roll technique eliminates that strain almost entirely.
To get out of bed: Roll your entire body as one unit onto your side, keeping your spine aligned and your core uninvolved. From that side-lying position, use your arms to push yourself upright while swinging your legs off the edge simultaneously. The arms do the work; the abdomen stays passive.
To get into bed: Sit on the edge of the mattress first, then lower your arms to the surface as you swing your legs up and roll onto your back as a single unit.
Practice this before surgery. It feels awkward the first few times, but it becomes instinctive quickly. Doing it correctly from day one protects your incision and dramatically reduces the discomfort of every bedtime and morning routine during recovery.

How Should You Build Your Sleep Setup Before an Appendectomy?
Here's the key insight that separates comfortable recoveries from miserable ones: don't try to figure out your sleep setup after surgery. The first days post-op are not the time for experimentation. You want your sleep environment assembled, tested, and ready to go before you leave for the hospital.
What Should Be in Place Before Surgery Day?
A wedge-based elevation system. The most important element. A proper upper body wedge creates the 30–45 degree incline essential for gas management, incision protection, and optimal healing. Stacked pillows are an unreliable substitute — they shift, compress under body weight, and rarely maintain the consistent angle a true wedge provides.
Knee elevation support. Elevating the legs gently takes additional pressure off the lower abdomen and lower back, which tends to accumulate strain when abdominal muscles aren't fully functional. A dedicated leg support wedge placed under the knees rounds out the body's support angles and reduces compensatory tension.
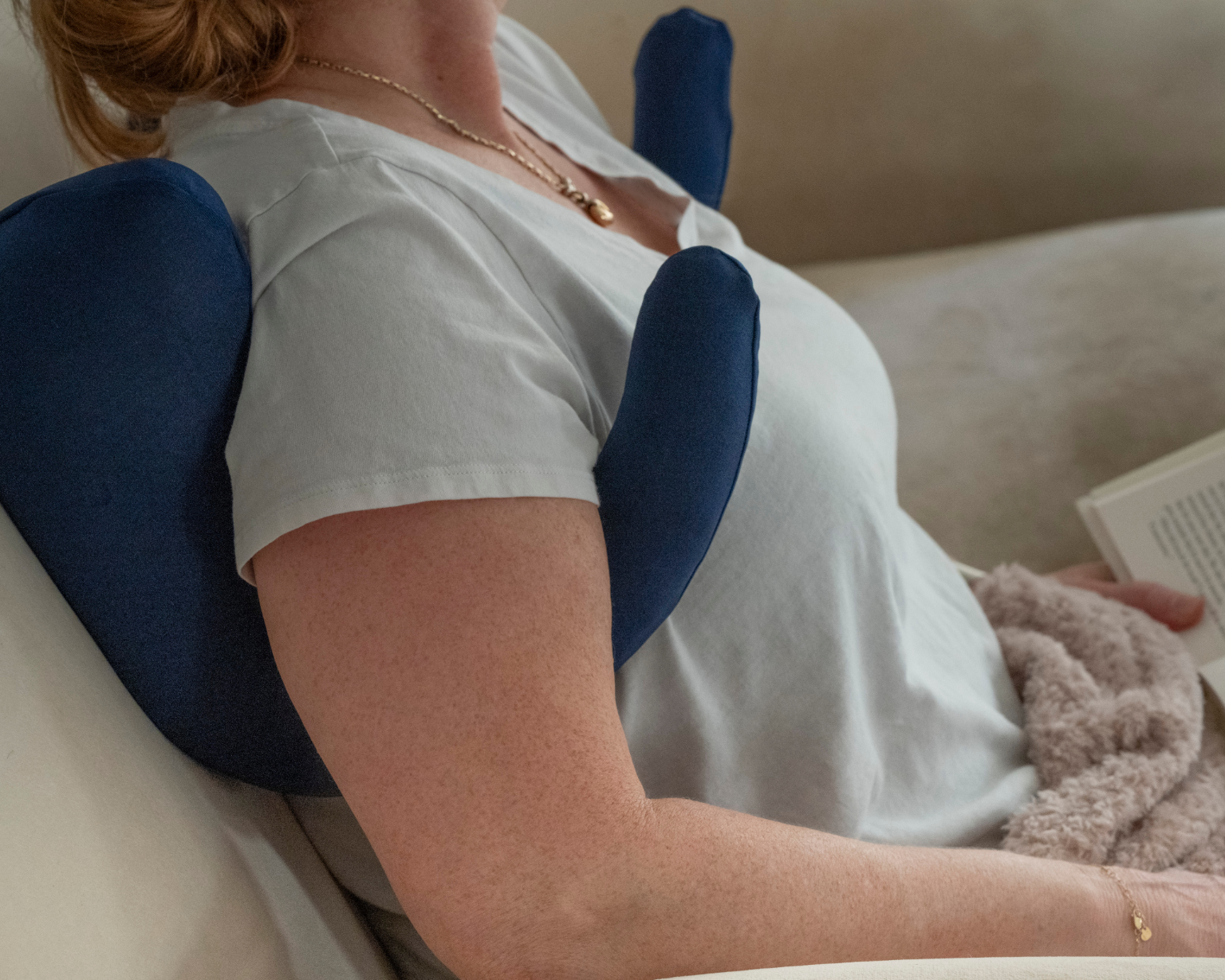
Side-cradling support. Even committed back sleepers shift during the night. Contoured pillows along both sides of the body act as physical boundaries that guide you back toward the center, reducing the chance of an uncomfortable and potentially painful overnight roll.
Head and neck support. Once your upper body is inclined, standard flat pillows don't provide adequate neck support at the elevated angle. A pillow designed for use with an upper body wedge maintains comfortable head position and natural neck mobility — and keeps everything you need for the night within arm's reach so you're never forced into a trunk-engaging reach or sit-up.
What Does a Week-by-Week Recovery Sleep Timeline Look Like?
Recovery isn't linear, but it does follow a predictable arc. Here's what to expect from your sleep positioning needs at each phase:
Days 1–7: Foundation Phase. This is the most important window for proper positioning. Gas-related discomfort peaks in the first 72 hours and gradually subsides. The 30–45 degree back-sleeping position should be your primary and essentially exclusive sleeping position during this phase. Prioritize consistency. Occasional elevated nights don't provide the same therapeutic benefit as sustained positioning.
Days 7–14: Transition Phase. Gas discomfort is largely resolved. Incision sites are actively healing but still tender. Continue elevated back sleeping as your primary position. If your surgeon has given the go-ahead, cautious left-side sleeping with knee support can be introduced — but return to back sleeping if you experience discomfort.
Weeks 2–4: Progression Phase. Most laparoscopic appendectomy patients are cleared for gradually broader position options in this window. Continue to avoid direct right-side sleeping and stomach sleeping. Elevation can be reduced incrementally as comfort allows. Full recovery — including a return to stomach sleeping if that's your preference — typically takes four to six weeks.
What If I Had an Open Appendectomy?
Open appendectomy patients face a meaningfully different recovery timeline than their laparoscopic counterparts.
The single larger incision, typically 2–4 inches, cuts through more layers of abdominal muscle and tissue, requiring a longer healing window before those muscles can safely bear load or tolerate positional stress.
Expect the elevated back-sleeping requirement to extend to three to four weeks minimum, with right-side and stomach sleeping off the table until your surgeon explicitly clears them, often not until the six to eight week mark.
The 30–45 degree elevation principle remains the same; the timeline for relaxing it is simply longer. If you had a ruptured appendix requiring open surgery, err on the side of caution with every positioning transition and follow your surgical team's guidance closely.

What Is the Sleep Again Pillow System, and How Does It Support Appendectomy Recovery?
Surgery recovery positioning systems take the guesswork out of everything described above. Rather than sourcing individual wedges, knee pillows, and support bolsters separately — and hoping they work together — an integrated system provides every element in a coordinated package designed specifically for post-surgical inclined back sleeping.
The Sleep Again Pillow System was designed around exactly the kind of multi-component support that appendectomy recovery requires. Every piece works together to create and maintain the therapeutic elevated back-sleeping position from day one of recovery.
Every Sleep Again Pillow System includes:
-
Two Contoured Side Pillows to cradle back and hips, providing the lateral boundaries that keep you comfortably positioned throughout the night
-
Upper Body Wedge to create the optimal upper body incline that drives gas relief, reduces swelling, and protects your healing incision
-
Leg Support Wedge to gently elevate the legs, reducing lower abdominal strain and improving overall circulation
-
Head Pillow to provide head support and neck mobility at the elevated sleeping angle
-
Removable, washable slipcovers for every piece, because recovery is messy and maintaining a clean sleep environment matters
GET BETTER SLEEP AFTER AN APPENDECTOMY

How Does Each Component Address Appendectomy Recovery Specifically?
The Upper Body Wedge is the cornerstone. It creates a sustained 30–45 degree incline that standard pillows cannot maintain through the night, keeping CO₂ gas migrating away from the diaphragm continuously rather than just at the moment you fall asleep, while holding abdominal muscles in their relaxed, shortened state.
The Two Contoured Side Pillows eliminate the involuntary rolling problem. Critical for anyone whose natural sleep position is the right side, directly over the surgical area, these pillows create a stable physical boundary that maintains your position without any conscious effort.
The Leg Support Wedge reduces lower abdominal tension and supports venous return to healing tissue.
The Head Pillow provides proper cervical alignment at the elevated angle the wedge creates — without it, the neck compensates awkwardly for the incline. And the removable, washable slipcovers on every piece keep the sleep environment clean through weeks of continuous recovery use.
This integrated approach addresses every positioning challenge an appendectomy patient faces — from CO₂ gas management in the early days to sustained incision protection through the full recovery arc — without requiring you to engineer a solution from scratch while you're in pain.
GET THE BEST PILLOW FOR APPENDECTOMY RECOVERY
Is the Sleep Again Pillow System Eligible for HSA/FSA?
Yes. The Sleep Again Pillow System qualifies as an HSA/FSA-eligible expense, making it a cost-effective addition to your pre-surgery preparation. If you have a Health Savings Account or Flexible Spending Account, check with your benefits administrator to confirm your specific plan's coverage. Using pre-tax dollars to fund a recovery tool that directly supports your surgical healing is the kind of practical planning that pays off immediately.
Please note: as bedding products, the Sleep Again Pillow System is not returnable under federal regulations, and all sales are final. This makes pre-surgery planning particularly valuable — purchasing and setting up your system before the procedure ensures you're confident in your setup from the moment you're home.

Frequently Asked Questions About Sleeping After an Appendectomy
Why use an integrated system like the Sleep Again Pillow System instead of assembling pillows myself?
The core challenge with a DIY pillow setup for appendectomy recovery is consistency. Standard pillows compress under body weight and shift during the night, which means the therapeutic 30–45 degree incline you set up at bedtime may not be the angle you're actually sleeping at by hour three. The Sleep Again Pillow System is purpose-built to maintain its positioning geometry through the night. Beyond consistency, the system addresses every component of the recovery position simultaneously — upper body incline, leg elevation, lateral support, and head positioning — in a coordinated package rather than a collection of mismatched pieces. For a recovery where positioning directly impacts healing speed and comfort, that reliability matters.
What is the best sleeping position after an appendectomy?
Elevated back sleeping at 30–45 degrees is the clinically recommended position for appendectomy recovery. This angle reduces CO₂ gas discomfort, protects your incision, supports lymphatic drainage to minimize swelling, and keeps abdominal muscles relaxed during healing. Adding leg elevation completes the support picture.
How long do I need to sleep elevated after an appendectomy?
Most laparoscopic appendectomy patients benefit from elevated back sleeping for the first 10–14 days, with gradual return to normal positions over four to six weeks. Open appendectomy recovery typically requires a longer positioning commitment. Always follow your surgeon's specific guidance — these timelines can vary based on complexity and individual healing.
Can I sleep on my side after an appendectomy?
Not in the first 7–10 days, and only cautiously after that. The right side puts direct pressure on the surgical area and should be avoided until your surgeon clears it. Left-side sleeping with a knee pillow is generally better tolerated once the early phase passes. Elevated back sleeping remains the most protective position throughout.
Why does my shoulder hurt after a laparoscopic appendectomy?
Residual CO₂ gas irritates the diaphragm, and the referred pain travels to the shoulder via the phrenic nerve. It typically resolves within 24–72 hours and is significantly reduced by sleeping elevated at 30–45 degrees rather than flat.
How do I stop rolling onto my incision at night?
The most effective approach is using contoured side pillows that physically prevent overnight rolling. Positioned along both sides of your body, they create a gentle boundary that guides you back toward the center during normal sleep movement. This eliminates the jarring awakenings that come with inadvertent position changes during recovery.
When can I return to sleeping on my stomach after an appendectomy?
Stomach sleeping is generally the last position cleared after abdominal surgery — typically at the four to six week mark for laparoscopic appendectomy, and potentially longer for open surgery. Your surgeon will confirm when abdominal healing has progressed sufficiently to tolerate the compression that stomach sleeping creates.
Can I use my HSA or FSA to buy recovery pillows?
The Sleep Again Pillow System qualifies as an HSA/FSA-eligible medical expense. If you're planning ahead for appendectomy recovery, your health savings account may cover the investment. Confirm with your plan administrator for specifics.
Final Thoughts: Plan Your Sleep Before Surgery, Not After
The most comfortable appendectomy recoveries share a common thread: the sleep setup was planned and in place before surgery day, not assembled afterward. When you're home from the hospital, sore, tired, and working around incisions, ordering wedge pillows that won't arrive for three days is not a recovery strategy.
The proactive approach is straightforward. Before surgery, identify your sleep setup. Understand why elevated back sleeping at 30–45 degrees works — not just that it's recommended, but the biomechanical reasons it matters for gas management, incision protection, and healing speed. Assemble your positioning tools. Have them in place, on your bed, ready to use the moment you walk back in the door.
If you're looking for a comprehensive solution that covers every piece of that setup in one package, the Sleep Again Pillow System was designed specifically for post-surgical recovery positioning. It addresses every element of the elevated back-sleeping position — the upper body wedge, the leg elevation, the lateral support, and the head positioning — with purpose-built components that work together rather than requiring individual trial and error.
Appendectomy recovery is temporary. A few weeks of intentional sleep positioning lead to a significantly more comfortable recovery and a faster return to normal life. Give your body the support it needs while it does the hard work of healing — it will make a real difference.
Important Medical Disclaimer
The information provided on this page is for educational purposes only and should not replace professional medical advice from your healthcare provider. Sleep Again Pillows are positioning support products designed to help maintain sleep positions recommended by medical professionals during recovery and for therapeutic use.
Always follow your surgeon's or physician's specific post-operative instructions and positioning requirements. Medical guidance from your healthcare team takes precedence over any general information provided here. Recovery timelines, positioning angles, and product suitability vary based on individual surgical procedures, medical conditions, and patient-specific factors.
Consult your healthcare provider before purchasing positioning equipment if you have specific medical concerns or questions about whether these products are appropriate for your recovery or medical condition(s). Your medical team can provide personalized recommendations based on your unique situation.
Sleep Again Pillows do not diagnose, treat, cure, or prevent any medical condition. These products provide positioning support to help maintain sleep angles and positions as directed by your healthcare provider.