Here's something that often catches people off guard before open heart surgery: sleep is one of the hardest parts of recovery, and one of the least prepared for.
Most pre-surgery conversations focus on the procedure itself, the hospital stay, and getting home safely. Sleep logistics rarely come up until patients are already home, uncomfortable, and trying to figure it out in real time.
This guide covers everything you need to know about sleeping positions after open heart surgery, why certain positions are off-limits (and for how long), and how the right tools can make all the difference between a difficult recovery and one where rest is genuinely working for you.
Why Sleep Is a Non-Negotiable Part of Cardiac Recovery
Sleep isn't just a nice-to-have during recovery. It's where the actual healing happens.
When you're asleep, your body releases growth hormone, consolidates immune function, reduces inflammation, and repairs tissue. After a surgery as significant as open heart surgery, that healing time is critical.
Research consistently shows that poor sleep quality after cardiac surgery is associated with longer recovery times, increased pain sensitivity, a higher risk of depression, and complications with wound healing. In other words, sleep quality isn't separate from your cardiac recovery. It is your cardiac recovery.
The challenge, of course, is that open heart surgery makes sleeping genuinely difficult, at least at first. Between the pain, the positioning restrictions, and the adjustment to being home after a major procedure, sleep after open heart surgery requires a plan.
Let's talk about that strategy.
What Open Heart Surgery Actually Does to Your Body (Sleep-Wise)
To understand why your sleeping position matters so much, you need to understand what happens during a typical open heart surgery, specifically a sternotomy.
A sternotomy is the most common surgical approach for procedures like bypass surgery, valve repair or replacement, and heart transplants. Once the surgery is complete, your sternum will take approximately 6 to 8 weeks to heal enough for you to resume normal activity.
Here's what that means for sleep:
-
Your chest wall is structurally compromised. Twisting, rolling, or putting pressure on your sternum can interfere with healing and, in severe cases, can cause sternal instability or wound separation.
-
Lying flat can increase the feeling of pressure on your chest and make breathing uncomfortable, especially in the early weeks.
-
Getting in and out of bed requires careful technique to avoid using your chest muscles or putting pressure on your sternum with your arms.
-
Side sleeping — the default position for approximately 74% of adults — is generally off-limits until your surgical team clears you, typically at the 6-to-8-week mark.
The bottom line: for the first phase of your recovery, you're a back sleeper. And not just any back sleeper but an inclined back sleeper.

Phase 1: Back Sleeping With Elevation (Weeks 1–6)
For most open heart surgery patients, the first six weeks of recovery are spent sleeping on their back in a slightly elevated position, typically 30 to 45 degrees.
Why the incline? A few reasons:
Easier breathing. After a sternotomy, lying completely flat can feel like a weight is sitting on your chest (because, functionally, something is — gravity and the pressure of your own ribcage). A gentle incline takes that pressure off, makes breathing easier, and reduces fluid buildup around the lungs, which is common post-surgery.
Less strain on your incision. An incline reduces the tension on your chest wall, which helps with both pain management and healing.
Reduced risk of acid reflux. Anesthesia and pain medications are rough on the digestive system. Elevation helps keep things where they belong.
Better circulation. Slight elevation supports venous return and reduces dependent edema — the uncomfortable swelling in the lower extremities that can accompany prolonged bed rest.
Why a Pile of Pillows Doesn't Cut It
Here's where most patients run into trouble early: trying to recreate an incline by stacking pillows. It's a reasonable instinct, but it doesn't hold up in practice.
Stacked pillows shift, flatten, and migrate throughout the night. They don't provide lateral support, which means rolling to your side remains a real risk. They don't support your arms, leaving them without a resting point. And coming out of alignment during the night after a sternotomy sets back both comfort and healing.
What you actually need is a support system that holds its position all night, keeps you inclined, prevents you from rolling, and supports your arms so that your chest muscles — which need to rest, not work — aren't bearing the load.

The Sleep Again Pillow System: Built for Open Heart Surgery Recovery
The Sleep Again Pillow System was designed by a breast cancer survivor who understood what post-surgical sleep actually requires. It has since become a go-to resource for people recovering from a wide range of surgeries, including open heart surgery, and for good reason.
Every Sleep Again Pillow System includes:
-
Two Contoured Side Pillows to cradle the back and hips and prevent rolling onto the side while sleeping
-
Upper Body Wedge to create optimal upper body incline
-
Leg Support Wedge to gently elevate legs
-
Head Pillow to provide head support and neck mobility
-
Removable, washable slipcovers for every piece
-
NEW - Set of Pillow Straps with Clasp (3-pk) now included!
For open heart surgery recovery, the Sleep Again Pillow System essentially solves every major sleep challenge of Phase 1 in one setup:
-
✓ Maintains an inclined position throughout the night
-
✓ Prevents rolling to either side
-
✓ Supports arms so chest muscles can rest
-
✓ Keeps the system stable on your mattress
-
✓ HSA/FSA eligible
Many patients use the Sleep Again Pillow System from the moment they arrive home from the hospital through the full duration of their sternal restriction period.
GET THE SLEEP YOU NEED DURING HEART SURGERY RECOVERY
The Art of Getting In and Out of Bed
Before we move on to Phase 2, let's talk about something that affects every sleeping position: getting in and out of bed.
This is underestimated by almost every open heart surgery patient. After a sternotomy, you cannot push off the bed with your hands or use your arm strength to prop yourself up. Your chest muscles are directly connected to your sternum, and engaging them puts stress on your incision.
Be sure to watch our setup video on tips for safely getting in and out of the system.
Phase 2: Transitioning Back to Side Sleeping (Weeks 6–12+)
At some point, typically around the 6-to-8-week mark, when your surgeon clears you, you can begin transitioning back to side sleeping. For most patients, this is a welcome milestone.
But the transition takes adjustment. After weeks of back sleeping, returning to side sleeping is not always immediately comfortable. Even when the sternum is healed, many patients experience:
-
Lingering tenderness and tightness along the incision line
-
Sensitivity across the entire chest wall, especially when pressure is applied
-
Anxiety about putting any weight on their chest — even when it's technically safe to do so
-
Discomfort from the chest wall and ribs resting on the mattress or arm
Finding a comfortable side sleeping position during this period is one of the more common challenges of cardiac recovery.

Enter the Side Sleeping Chest Pillow: Perfect for Transitioning Back to Side Sleeping After Open Heart Surgery
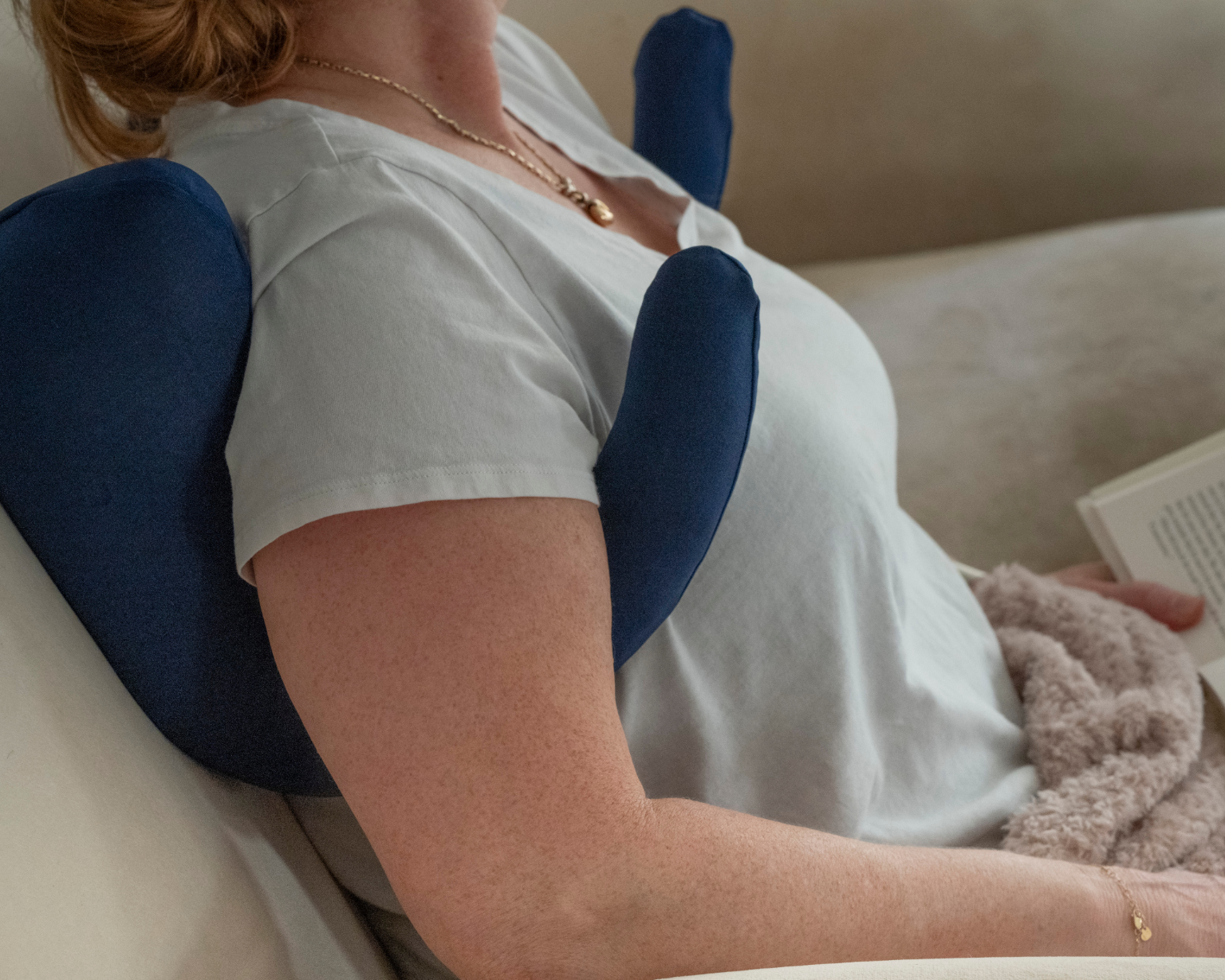
The Side Sleeping Chest Pillow was specifically designed to solve the problem of chest tenderness and sensitivity during the transition back to side sleeping.
Here's how it works:
The pillow has a butterfly/U-shaped design with two cushioned sides and an adjustable connecting strap. When you lie on your side, the two sides cradle your chest from the front and support your back simultaneously, creating a supported "nest" that prevents your chest from collapsing directly onto the mattress.
What makes it particularly smart:
Adjustable width. The strap connecting the two sides is adjustable, so you can position the cushions to perfectly cradle your chest, accounting for your specific body shape, incision placement, and sensitivity level.
Symmetrical design. You can sleep on either side without flipping the pillow or readjusting. Both sides are supported equally, which means you can turn freely during the night as your comfort dictates — a huge deal when you've been locked into one position for weeks.
Wedge-shaped cushions. The sides of the pillow have a gentle wedge shape, giving you flexibility in how much support you need. Position them closer together for more support or further apart for less, depending on where you are in your recovery.
Compact and unobtrusive. Unlike large body pillows, the Side Sleeping Chest Pillow sits under your waist area and doesn't take over the bed. You can make your bed in the morning and simply leave it in position for that night.
Price point and eligibility. At $45 and HSA/FSA eligible, it's an accessible addition to your recovery toolkit — especially given how much it can improve sleep quality during what is otherwise a frustrating transition.
For open heart surgery patients, the Side Sleeping Chest Pillow bridges the gap between Phase 1 (full back sleeping with the Sleep Again Pillow System) and full, unrestricted side sleeping. Many patients find they use it well beyond the 8-week mark, especially those with a naturally sensitive chest wall or those who had more complex procedures.
SLEEP ON YOUR SIDE SAFELY AFTER OPEN HEART SURGERY
Important note: Always follow your surgeon's directions regarding when its safe to sleep on your side after heart surgery, and do not attempt side sleeping until you are cleared to do so.
Sleeping Positions to Avoid After Open Heart Surgery
To be thorough: here's what your care team is almost certainly going to tell you not to do, and why.
Sleeping flat on your back (without elevation) — avoid for the first 2–4 weeks. Complete flat-back sleeping can increase the sensation of chest pressure, worsen shortness of breath, and increase fluid accumulation around the lungs. The inclined back sleeping position described above is much more comfortable and physiologically supportive.
Sleeping on your stomach — avoid for at least 8–12 weeks. Prone sleeping puts direct pressure on your sternum and is completely contraindicated after sternotomy. Don't even attempt it until you have explicit clearance from your surgeon.
Sleeping on your side — avoid for 6–8 weeks, or until cleared. Even if it feels okay, your sternum needs to be fully healed before your body weight is applied laterally to your chest wall. Side sleeping too early is one of the most common reasons patients experience sternal complications.
Sleeping in a recliner for extended periods. Some patients default to sleeping in a recliner because it's already inclined and they don't have to deal with getting in and out of bed. While a recliner can work in a pinch, it's not a long-term solution. It doesn't provide adequate support for your body, can cause hip and back pain, and often leads to worse sleep quality overall. A proper inclined back-sleeping setup in your bed, like the Sleep Again Pillow System, is a significantly better option.

Pre-Surgery Sleep Prep: The Smart Play
One of the most empowering things you can do before your surgery is prepare your sleep environment in advance. This is proactive recovery in action — and it's one of the areas where small investments before surgery pay massive dividends during recovery.
Here's a pre-surgery sleep prep checklist:
1. Set up your Sleep Again Pillow System before your surgery date. Have it assembled and ready. Sleep in it a few nights before surgery if possible, so the transition home isn't jarring. Learn more about the system.
2. Have the Side Sleeping Chest Pillow on hand. You won't need it right away, but having it ready for the 6-week transition point means it's there when you need it. At $45, it's a practical addition to have on hand before surgery. Learn more about the Side Sleeping Chest Pillow.
3. Adjust your bed height, if possible. The ideal bed height for open heart surgery recovery is one where your feet touch the floor when you're sitting on the edge, with your hips at approximately 90 degrees. If your bed is too low, consider a bed riser. If it's too high, a stool may help. You might be interested in our setup videos to learn more about what to expect and how our system works.
4. Clear the path. Make sure your path from bed to bathroom is clear of obstacles, well-lit for nighttime trips, and free of anything that requires stepping over or around. Mobility will be limited during the early weeks of recovery.
5. Educate your caregivers. Your partner, family members, or caregivers should know how to assist you in getting in and out of bed without grabbing your arm or shoulder (which would engage your chest muscles).
6. Stock your nightstand. Water, your pain medication and schedule, your phone charger, a notepad for any symptoms you want to note — everything you might need overnight should be within arm's reach without requiring you to lean, twist, or get up unnecessarily.
Frequently Asked Questions: Sleeping After Open Heart Surgery
How long do I have to sleep on my back after open heart surgery?
Most cardiac surgeons recommend back sleeping for a minimum of 6 to 8 weeks post-sternotomy, with side sleeping clearance coming at a follow-up appointment. Follow your surgical team's guidance on timing rather than going by how you feel — sternal healing isn't always outwardly symptomatic.
Can I sleep in a recliner after open heart surgery?
A recliner can be ok for short daytime naps or TV watching, but it's not a long-term solution. See the "Sleeping Positions to Avoid" section above for the full breakdown on why a proper in-bed setup wins out.
Will I always have to sleep on my back after open heart surgery?
No. Once your sternum is healed and you've been cleared by your surgeon, you can return to your preferred sleeping position. The Side Sleeping Chest Pillow is specifically designed to ease this transition if your chest feels tender or sensitive as you work your way back to side sleeping.
Why is getting in and out of bed so hard after open heart surgery?
After a sternotomy, you can't use your arms or chest muscles to push yourself up because doing so puts strain on your sternum. The log-roll technique (rolling as a unit to your side, then using leg momentum to rise) takes the chest out of the equation. A bed at the right height and consistent lateral support (like the side pillows in the Sleep Again Pillow System) makes this significantly easier.
My surgeon said I can sleep on my side. Why does it still hurt?
Even after your sternum has healed enough to be "cleared" for side sleeping, the surrounding tissue — muscles, fascia, skin — can remain sensitive for months. Many patients find that the direct pressure of lying on their side is uncomfortable, even when the bone itself is fine. The Side Sleeping Chest Pillow is built specifically for this gap: it reduces direct pressure on your chest wall and distributes support across both sides of your body so you can actually enjoy side sleeping again.
Is the Sleep Again Pillow System worth it just for recovery?
Short answer: yes, overwhelmingly. The alternative is weeks of interrupted sleep, chronic fatigue during your most vulnerable recovery period, and the real risk of compromising your healing by rolling onto your side in the night. Many users end up keeping it long after their recovery for its general comfort, as elevated back sleeping has numerous health benefits.
The Bottom Line: Sleep Is Part of Your Recovery Plan
Open heart surgery is one of the most significant physical events a human body can experience. And yet sleep — one of the most powerful recovery tools you have — is consistently underplanned for. Understanding sleeping positions after open heart surgery before your procedure gives you a meaningful advantage from day one at home.
You wouldn't show up to your surgery without understanding the procedure. Don't show up to your recovery without understanding how you're going to sleep.
The Sleep Again Pillow System gives you the inclined, laterally-supported, stable back-sleeping setup you need for Phase 1 — the critical first 6 to 8 weeks when your sternum is healing and rolling to your side isn't an option.
The Side Sleeping Chest Pillow gives you a gentle, adjustable bridge back to side sleeping when your surgeon clears you — so you're not starting from zero when it's time to reclaim your favorite sleep position.
Together, they cover the full arc of post-open-heart-surgery sleep recovery. Getting them in place before surgery means your rest — and your healing — starts on solid footing from day one.
Important Medical Disclaimer
The information provided on this page is for educational purposes only and should not replace professional medical advice from your healthcare provider. Sleep Again Pillows are positioning support products designed to help maintain sleep positions recommended by medical professionals during recovery and for therapeutic use.
Always follow your surgeon's or physician's specific post-operative instructions and positioning requirements. Medical guidance from your healthcare team takes precedence over any general information provided here. Recovery timelines, positioning angles, and product suitability vary based on individual surgical procedures, medical conditions, and patient-specific factors.
Consult your healthcare provider before purchasing positioning equipment if you have specific medical concerns or questions about whether these products are appropriate for your recovery or medical condition(s). Your medical team can provide personalized recommendations based on your unique situation.
Sleep Again Pillows do not diagnose, treat, cure, or prevent any medical condition. These products provide positioning support to help maintain sleep angles and positions as directed by your healthcare provider.